Corticotropin-releasing hormone induces proliferation and TNF-α release in cultured rat microglia...
Transcript of Corticotropin-releasing hormone induces proliferation and TNF-α release in cultured rat microglia...
Corticotropin-releasing hormone induces proliferation
and TNF-a release in cultured rat microglia via
MAP kinase signalling pathways
Wei Wang, Ping Ji and Kimberly E. Dow
Department of Pediatrics, Queen’s University, Kingston, Ontario, Canada
Abstract
We have previously demonstrated that corticotropin-releasing
hormone (CRH) receptor 1 (CRH-R1) is functionally
expressed in rat microglia. In the present study, we show that
CRH, acting on CRH-R1, promoted cell proliferation and
tumour necrosis factor-a (TNF-a) release in cultured rat
microglia. Exogenous CRH resulted in an increase in BrdU
incorporation compared with control cells, which was
observed in a range of concentrations of CRH between 10 and
500 nM, with a maximal response at 50 nM. The effect of CRH
on BrdU incorporation was inhibited by a CRH antagonist
astressin but not by a cAMP-dependent protein kinase inhib-
itor H89. Exposure of microglial cells to CRH resulted in a
transient and rapid increase in TNF-a release in a dose–
dependent manner. In the presence of astressin, the effects of
CRH on TNF-a release were attenuated. CRH effects on TNF-a
release were also inhibited by specific inhibitors of MEK, the
upstream kinase of the extracellular signal-regulated protein
kinase (ERK) (PD98059) or p38 mitogen-activated protein
kinase (SB203580), but not by H89. Furthermore, CRH induced
rapid phosphorylation of ERK and p38 kinases. Astressin,
PD98059, and SB230580 were able to inhibit CRH-induced
kinase phosphorylation. These results suggest that CRH
induces cell proliferation and TNF-a release in cultured micro-
glia via MAP kinase signalling pathways, thereby providing
insight into the interactions between CRH and inflammatory
mediators.
Keywords: cytokine, extracellular signal-regulated protein
kinase, glia, p38, receptor, signal transduction.
J. Neurochem. (2003) 84, 189–195.
Corticotropin releasing hormone (CRH), a 41-amino-acid
neuropeptide, plays a central regulatory role as a key
mediator of the hypothalamic-pituitary-adrenal system
response to stress (Vale et al. 1981; Owens and Nemeroff
1991; De Souza 1995). CRH elicits its biological effects by
binding to two G protein-coupled membrane receptors
(CRH-R1 and CRH-R2) with signal transduction being
mediated via several intracellular signalling pathways such as
cAMP, protein kinase C, and mitogen-activated protein
kinases (MAPK) (Chen et al. 1993; Lovenberg et al. 1995;
Perrin et al. 1995; Kostich et al. 1998; Li et al. 1998; Cibelli
et al. 2001). CRH receptors are widely distributed in the
central nervous system (CNS) in general concordance with
the distribution of CRH pathways (De Souza 1995). Recent
studies have also indicated a broad range of distribution of
CRH receptors in the immune, cardiovascular and reproduc-
tive systems, suggesting that the receptors may mediate many
diverse functions (Singh and Fudenberg 1988; Audhya et al.
1991; Clifton et al. 1995; Perrin et al. 1995). In addition to
its effects on hormone regulation, CRH has been implicated
in pathological and pathophysiological responses in various
neurodegenerative disorders, including brain traumatic,
ischemic and excitotoxic injuries. These neurodegenerative
disorders are accompanied by an increase in brain CRH and
its receptors (Wong et al. 1995; Greenwood et al. 1997; Roe
et al. 1998; Wang et al. 2000). Several lines of evidence
suggest that CRH contributes to neuronal loss in vitro and
in vivo while some studies show a protective role of CRH.
Received August 2, 2002; revised manuscript received October 22,
2002; accepted October 23, 2002.
Address correspondence and reprint requests to Dr Kimberly E. Dow,
Doran 3, Room 6–303, Apps Medical Research Center, Kingston Gen-
eral Hospital, Kingston, Ontario, Canada K7L 2V7, Canada.
E-mail: [email protected]
Abbreviations used: CREB, cAMP response element-binding protein;
CRH, corticotropin-releasing hormone; CRH-R1, corticotropin-releasing
hormone receptor 1; ERK, extracellular signal-regulated protein kinase;
GFAP, glial fibrillary acidic protein; LPS, lipopolysaccharide; MAPK,
mitogen-activated protein kinases; PKA, cAMP-dependent protein kin-
ase; TNF-a, tumour necrosis factor-a.
Journal of Neurochemistry, 2003, 84, 189–195
� 2003 International Society for Neurochemistry, Journal of Neurochemistry, 84, 189–195 189
(Strijbos et al. 1994; Maecker et al. 1997; Roe et al. 1998;
Lezoualc’h et al. 2000; Brunson et al. 2001; Pedersen et al.
2001). The molecular mechanisms of CRH effects and the
functional importance of CRH receptors during these stress-
related conditions are largely unknown. Some studies have
shown that increased CRH following brain insults plays an
important role in immunomodulation in either an autocrine or
paracrine manner at the level of the CNS (Karalis et al. 1991;
Vamvakopoulos and Chrousos 1994; Chrousos 1995; Der-
mitzaki et al. 2002).
Microglia, brain resident macrophages, play an important
role in immunoregulation in the CNS by interacting with
neurons, astrocytes, and other glial cells (Kreutzberg 1996;
Giulian 1987). Activated microglia are known to have both
restorative and cytotoxic capabilities by releasing a number
of inflammatory mediators such as nitric oxide, interleukines,
and cytokines (Merrill and Jonakait 1995; Kreutzberg 1996).
These inflammatory mediators, e.g. a potential neurotoxic
cytokine tumour necrosis factor-a (TNF-a) induced by brain
insult or by lipopolysaccharide (LPS), participate in regula-
ting inflammation, immune responses, neurotransmission,
and neural cell death/survival. Thus, microglia play a key
role in mediating CNS tissue damage, both in the early stage
of inflammation and the later stage of tissue repair.
Recently we have shown that functional CRH-R1 is
expressed in rat brain microglia (Wang et al. 2002). There-
fore, CRH may regulate microglial functions such as
inflammatory mediator release, by activation of the CRH
receptor in microglia. To further investigate the physiological
significance of such a receptor in microglia, we examined
whether exogenous administration of CRH regulates cell
proliferation and TNF-a release in primary cultures of rat
brain microglia. Because the release of inflammatory medi-
ators is believed to be mediated through signalling pathways
involving MAPKs, such as extracellular signal-related kin-
ases (ERK) and p38 kinase (Robinson and Cobb 1997), we
also examined effects of CRH on activation of ERK and p38
kinases and effects of inhibitors of ERK and p38 kinases on
CRH-regulated TNF-a release.
Materials and methods
Reagents
Peptide analogues (human/rat CRH and astressin) were purchased
from Bachem (Torrance, CA, USA). MEK1/2 inhibitor PD98059
and p38 kinase inhibitor SB203580 were obtained from Calbiochem
(San Diego, CA, USA). The peptide stock solution was prepared by
dissolving CRH in 0.01 N HCl/0.1% BSA in PBS and stored at
) 20�C. Astressin was dissolved in 0.01 N HCl/0.1% BSA in
distilled water and stored at ) 20�C. BrdU cell proliferation enzyme-
linked immunosorbent assay (ELISA) kit was purchased from
Boehringer Mannheim (Mannheim, Germany). Rat TNF-a ELISA
kit was purchased from Biosource International Inc. (Camarillo, CA,
USA). Anti-phospho-ERK (p44/p42) and anti-total ERK (p44/p42)
polyclonal antibodies were obtained from Cell Signaling (Beverly,
MA, USA) as were anti-phospho-p38 MAP kinase and anti-total
p38 MAP kinase antibodies. All other chemicals and reagents were
obtained from Sigma (St Louis, MO, USA).
Microglia cultures
Cultures of microglia were established based on the differential
adherence of cells harvested from embryonic rat cortex as described
previously (Wang et al. 2002). Briefly, mixed cell cultures were
established from E19 rat cerebral cortex. Cortices were dissociated
by passing through a 70-mm Nitex mesh and plated in culture flasks.
Cultures were fed every 4 days with Dulbecco’s modified Eagle’s
medium (DMEM)/F12 containing 10% foetal calf serum (FCS). On
day 12, the cultures were shaken for 10 min. The suspended cells
were plated on uncoated dishes or plates and incubated for 1 h at
37�C. The medium containing suspended cells was discarded and
adherent cells were fed with DMEM containing 10% FCS. Cultures
with cells positive for the astrocyte marker glial fibrillary acidic
protein (GFAP) or for the oligodendrocyte marker galactocerebro-
side were discarded (Wang et al. 2002).
Proliferation assay
Microglia were plated at 5 · 104 cells/well in 96-well plates and
incubated overnight in DMEM containing 10% FCS. Cultured
medium was changed to DMEM containing 0.1% FCS for a further
24 h. Cells were then treated with indicated concentrations of CRH
for 48 h. After exposure to CRH, cultures were analyzed for cell
proliferation by measuring BrdU incorporation using the BrdU cell
proliferation ELISA kit (Boehringer Mannheim) according to the
manufacturer’s instructions. Briefly, 10 lM BrdU was added to
culture medium 6 h before the end of CRH treatment. Then, culture
medium was removed and cells were fixed for 20 min at room
temperature (20�C). Anti-BrdU-antibody was added to wells and
incubated for 60 min and the wells were washed three times with
washing solution. The immune complexes were detected by the
subsequent substrate reaction and reaction products were quantified
by measuring the absorbance at 450 nm. The developed colour and
thereby the absorbance values directly correlated to the amount of
DNA synthesis and the number of proliferating cells.
Measurement of TNF-a release
Microglia were plated into 24-well plates at 2 · 105 cells/well and
incubated overnight. Cells were then treated with various concen-
trations of CRH for different times. TNF-a released into culture
media was measured using rat TNF-a ELISA kits (Biosource)
according to the manufacturer’s instructions. The final concentra-
tions of TNF-a were calculated by converting the optical density
readings using standard curves.
Measurement of ERK and p38 kinase phosphorylations
Western blots were performed for the analysis of ERK and p38
kinase phosphorylation. Briefly, cultured microglia were collected
and lysed in sample buffer and sonicated for 10–15 s. The samples
(80 lg of protein) were boiled for 5 min and electrophoresed on a
10% sodium dodecyl sulfate – polyacrylamide gel electrophoresis
(SDS–PAGE). After electrophoresis, gels were blotted to nitrocel-
lulose membranes. Following blocking with 5% non-fat milk, the
membranes were washed and incubated with primary antibodies
190 W. Wang et al.
� 2003 International Society for Neurochemistry, Journal of Neurochemistry, 84, 189–195
(phospho-p44/p42 and phospho-p38 kinase rabbit polyclonal anti-
bodies at a final concentration of 1 : 1000) overnight at 4�C.
Subsequently, the membranes were washed again and incubated
with HRP-conjugated secondary antibody (1 : 2000) and HRP-
conjugated antibiotin antibody (1 : 1000) for 1 h at room tempera-
ture. The bands were visualized by an enhanced chemiluminescence
detection system (Amersham Pharmacia Biotech, Piscataway, NJ,
USA). To normalize the results, membranes were stripped and
reprobed with antibodies specific for total p44/42 or p38 kinases,
respectively. Protein concentrations of samples were determined by
the method of Bradford using BSA as a standard (Bio-Rad
Laboratories, Hercules, CA, USA).
Statistical analysis
Differences between groups were compared by student’s t-test and
analysis of variance or by Kruskal–Wallis one-way analysis of
variance on ranks using SigmaStat software.
Results
Effect of CRH on proliferation of microglia
To investigate a possible role for CRH in microglia
proliferation, BrdU incorporation was measured as an index
of microglial proliferation. Microglia in DMEM containing
0.1% FCS were treated with indicated concentrations of
CRH, the CRH receptor antagonist astressin, or a combina-
tion of CRH and astressin. As shown in Fig. 1, CRH treated
cells showed an increase to �160% of the control levels in
BrdU incorporation over 48 h in culture. The CRH-induced
increase in BrdU incorporation was dose–dependent in the
concentration range of 10–200 nM and the microglial
response to CRH reached a plateau at 50 nM (Fig. 1). When
microglia were incubated in medium containing 10% serum,
CRH had no effect (data not shown). To study the specificity
of the stimulating effect of CRH on microglial proliferation,
cells were treated with CRH in the presence or absence of the
CRH receptor antagonist astressin. The effect of CRH on
BrdU incorporation was inhibited by 200 nM astressin
(Fig. 2a). Astressin alone at 200 nM did not alter the basal
level of BrdU incorporation.
As activation of CRH receptors is classically associated
with activation of the cAMP-dependent protein kinase (PKA)
pathway, cells were treated with the PKA inhibitor H89 at
30 lM for 1 h before addition of CRH. The effect of CRH on
BrdU incorporation was not attenuated by the presence of
H89 (Fig. 2b).
CRH and its related peptides have been shown to activate
MAP kinase signal transduction pathways and phosphoryla-
tion of the transcription factor calcium/cAMP response
element-binding protein (CREB) in several cell types (Li
et al. 1998; Rossant et al. 1999; Cibelli et al. 2001). The
regulation of cell proliferation is correlated with the activa-
tion of MAP kinases, especially the ERK subgroup (Peletch
and Sanghera 1992; Tournier et al. 1994). The role of MAP
kinase in CRH-induced microglial proliferation was inves-
tigated by using an inhibitor of MEK, an upstream kinase of
ERK1/2, PD98059. This inhibitor at a concentration of
50 lM significantly inhibited CRH-induced proliferation
Fig. 1 Effect of CRH on cell proliferation in microglia. Microglia were
incubated with indicated concentrations of CRH in DMEM containing
0.1% FCS for 48 h. Cell proliferation was measured by BrdU incor-
poration ELISA. Results are taken from three independent cultures
and experiments. Data are mean ± SD. *p < 0.05 versus control.
Fig. 2 Effect of astressin (a), H89 or PD98059 (b) on CRH-induced
proliferation. Microglia were incubated with the CRH antagonist
astressin (AS, 200 nM), PKA inhibitor H89 (30 lM) or ERK1/2 inhibitor
PD98059 (PD, 50 lM) for 1 h prior to addition of 100 nM of CRH. Cell
proliferation was determined 48 h following CRH treatment. Results
are taken from three independent cultures and experiments. Data are
mean ± SD. *p < 0.05 versus control, **p < 0.05 versus CRH.
CRH induces TNF-a release in microglia 191
� 2003 International Society for Neurochemistry, Journal of Neurochemistry, 84, 189–195
when incubated with cells for 1 h prior to the addition of
CRH (Fig. 2b).
CRH induces TNF-a release in microglia
To study the effect of CRH on TNF-a release in cultured rat
microglia, microglial cells were treated with the indicated
concentrations of CRH for different times and TNF-a release
into the culture medium was determined. Basal levels of
TNF-a in untreated microglia were low and CRH treatment
induced an increased release of TNF-a compared with
control cells (Fig. 3a). A dose–dependent increase in TNF-arelease by CRH was seen up to 250 nM, with the peak
response at 100 nM (Fig. 3a). The time course of CRH-
induced TNF-a release was determined at 2, 4, 6, 24, and
48 h following CRH treatment. As shown in Fig. 3b,
increased release of TNF-a was detected at 2 h after the
addition of CRH. The peak increase of TNF-a release was at
4 and 6 h and then returned to basal levels at 24 h (Fig. 3b).
The marked decrease of TNF-a release at 24 h could largely
be due to the degradation of TNF-a in the culture medium.
Receptor binding of soluble TNF-a could be a contributing
factor (Pyo et al. 1999; Jana et al. 2002). The effect of CRH
on TNF-a release was attenuated when cells were treated
with 200 nM of astressin for 1 h prior to CRH treatment
(Fig. 4a).
To study whether the cAMP-dependent mechanism is
associated with the effect of CRH on TNF-a release, CRH-
induced TNF-a release was determined in the presence or
absence of H89. H89 at a concentration of 30 lM, when
added to cell cultures for 1 h prior to the addition of CRH,
did not alter CRH-induced TNF-a release (Fig. 4b).
To test whether MAP kinase signalling pathways are
involved in the effect of CRH on TNF-a release, microglial
cells were treated with upstream inhibitor of ERK (PD98059)
or p38 kinase (SB203580) at concentrations of 50 lM for 1 h
prior to the addition of CRH and TNF-a release was
determined. Both PD98059 and SB203580 inhibited the
effect of CRH on TNF-a release (Fig. 5). When both
inhibitors were used simultaneously, TNF-a levels were
further decreased (Fig. 5).
CRH induces activation of ERK and p38 MAP kinases
To further investigate the role of MAP kinase signalling
pathways in CRH-induced TNF-a release, microglial cells
were treated with CRH and the phosphorylation status of
ERK and p38 kinases were analyzed by western blotting
using commercially available antibodies specific for the
active forms of the two kinases. As shown in Fig. 6, CRH
Fig. 4 Effects of astressin (a) or H89 (b) on CRH-induced TNF-a
release. Microglia were pre-treated with the CRH antagonist astressin
(AS, 200 nM) or H89 (30 lM) for 1 h prior to addition of 100 nM of CRH.
TNF-a release was determined at 4 h following CRH treatment.
Results are taken from three independent cultures (n ¼ 18). Data are
mean ± SD. *p < 0.05 versus control, **p < 0.05 versus CRH.
Fig. 3 CRH induced TNF-a release in cultured microglia. Microglia
were treated with (a) indicated concentrations of CRH for 4 h or
treated with (b) 100 nM of CRH for indicated time periods. Amounts of
TNF-a released were determined by TNF-a ELISA. Results are taken
from three independent cultures (n ¼ 18). Data are mean ± SD.
*p < 0.05 versus control.
192 W. Wang et al.
� 2003 International Society for Neurochemistry, Journal of Neurochemistry, 84, 189–195
induced a transient phosphorylation of both ERK and p38
kinases. The maximal activation of ERK and p38 kinases by
CRH was observed after 20–30 min (Fig. 6). After being
stripped, the membranes were reblotted with anti-total-p44/
42 or p38 antibodies. Normalizing with non-phosphorylated
forms of p44/42 and p38 kinases confirmed that CRH
specifically altered p42/44 and p38 kinase phosphorylation,
but not expression levels. The effect of CRH on ERK and
p38 phosphorylation was inhibited by 200 nM astressin
(Fig. 6). PD98059 at 50 lM significantly inhibited the CRH
effect on ERK kinase phosphorylation when incubated with
cells for 1 h prior to the addition of CRH (Fig. 6). In a
similar manner, the p38 kinase inhibitor SB203580 at 50 lM
also inhibited CRH-induced phosphorylation of p38 kinase
(Fig. 6). Neither PD98059 nor SB203580 had any effect on
cell viability in a concentration range of 1–100 lM (data not
shown). These results suggest that activation of ERK and p38
MAP kinase pathways by CRH is necessary to trigger TNF-arelease in cultured microglia.
Discussion
We have recently demonstrated the functional expression of
CRH-R1 in cultured microglia of rat brain (Wang et al.
2002). In the present study, we extended our previous
observations on the biological response of microglia to CRH.
Our results suggest that (i) CRH promoted cell proliferation
and induced TNF-a release from cultured microglia via
activation of CRH-R1, (ii) CRH-induced microglial prolif-
eration and TNF-a release were associated with activation of
both ERK and/or p38 MAP kinase signalling pathways, and
(iii) the effects of CRH appeared to be independent of
cAMP-dependent protein kinase pathways.
CRH has been shown to promote or inhibit cell prolifer-
ation via interacting with CRH-R1 in several cell types
(McGillis et al. 1989; Singh 1989; Ha et al. 2000; Carlson
et al. 2001; Mitsuma et al. 2001; Quevedo et al. 2001).
CRH promotes proliferation in developing astrocytes in
cerebellar cultures, an effect which is thought to be mediated
through the cAMP pathway and activation of c-Fos (Ha et al.
2000). In malignant melanoma cells, CRH inhibits prolifer-
ation via activation of CRH-R1 and subsequently altered
intracellular Ca2+ signalling (Carlson et al. 2001). The
results of the present study showed that CRH promoted
microglial proliferation and that the CRH effect was inhibited
by astressin, suggesting involvement of the activated CRH
receptor expressed in microglia. The effect of CRH on
microglial proliferation appears to involve MAP kinase
signalling and is independent of cAMP-PKA pathways. The
mechanisms for the effects of CRH on proliferation are not
yet clear, but may depend on cell types and differential signal
pathways activated.
Fig. 5 Effects of ERK and p38 kinase inhibitors on CRH-induced TNF-a
release. Microglia were incubated with PD98059 (PD, 50 lM) or
SB203580 (SB, 50 lM) for 1 h prior to addition of CRH (100 nM). TNF-a
released was determined at 4 h following CRH treatment. Results are
taken from three independent cultures (n ¼ 18). Data are mean ± SD.
*p < 0.05 versus control, **p < 0.05 versus CRH.
(a) (b)
(c) (d)
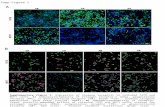
Fig. 6 CRH induced phosphorylation of
ERK (a) and p38 kinases (b). Microglia
were treated with 100 nM of CRH for indi-
cated time periods and phosphorylation
status of ERK and p38 kinases were
analyzed by western blot as described in
Materials and methods. Experiments were
done from three independent cultures.
A representative experiment is shown.
Panels (c) and (d) showed the effect of
astressin (AS, 200 nM), PD98059 (PD,
50 lM) or SB203580 (SB, 50 lM) on CRH-
induced ERK and p38 kinases activation.
CRH induces TNF-a release in microglia 193
� 2003 International Society for Neurochemistry, Journal of Neurochemistry, 84, 189–195
Studies have suggested that CRH plays a role in immune
function by promoting immune cells to produce inflamma-
tory mediators (Singh and Leu 1990; Angioni et al. 1993).
Our data provide evidence that CRH-induced TNF-a release
from cultured microglia is mediated by activation of the
MAP kinase pathways. It has been demonstrated that CRH
and its related peptides can activate ERK and p38 kinases in
several cell types (Li et al. 1998; Rossant et al. 1999; Cibelli
et al. 2001; Dermitzaki et al. 2002). In the present study, an
increase in tyrosine phosphorylation of ERK and p38 kinases
was detected within 30 min following treatment with CRH.
CRH-induced phosphorylation of ERK and p38 kinases was
inhibited by MEK/ERK (PD98059) and p38 (SB203580)
kinase inhibitors, respectively. The activation of ERK and
p38 was also blocked by the CRH receptor antagonist
astressin. Furthermore, CRH-induced TNF-a release from
microglia was reduced by pre-treatment with both PD98059
and SB203580. While a recent report has shown that CRH
can activate p38 MAPK (Dermitzaki et al. 2002), SB203580
may also inhibit c-Raf, an upstream form of the p44/42 MAP
kinase (Hall-Jackson et al. 1999). Thus, SB203580 may
have its inhibitory effect by acting through p44/42 MAP
kinase. Further studies are required to provide direct
evidence for the involvement of p38 in CRH-induced cell
proliferation and TNF-a release. While we have recently
shown that CRH increases cAMP levels in cultured microglia
(Wang et al. 2002), modulation of cell proliferation and
TNF-a release by CRH may not require the activation of the
cAMP-PKA pathway. Thus the diverse functions of CRH in
the brain and peripheral tissues may be due in part to the
selective activation of these two downstream signal path-
ways.
The immune and neuroendocrine systems are two essential
physiological components linked by reciprocal regulatory
interactions. CRH has been shown to modulate inflammatory
responses by regulating the pro- or anti-inflammatory
mediators at the level of the CNS (Sapolsky et al. 1987;
Karalis et al. 1991; Angioni et al. 1993; Vamvakopoulos and
Chrousos 1994; Chrousos 1995; Paez Pereda et al. 1995;
Linthorst et al. 1997). In light of microglial function in the
CNS, the present results demonstrate a potentially important
function of CRH in both normal homeostasis and neurode-
generative disease states. Therefore, our findings may
provide insight into basic cellular interactions between
CRH and inflammatory mediators in pathological conditions
within the CNS. The interaction may prove to be a very
important mechanism in responses to stressful challenges
such as acute or chronic brain insults.
Acknowledgements
This work was supported by the Principal’s Developmental Fund of
Queen’s University (380–006 to WW) and the Angada Foundation
(365–983 to WW) and in part by the Heart and Stroke Foundation of
Ontario (NA5024 to KED). We thank Dr G. Zhao for his technical
assistance in microglia cultures.
References
Angioni S., Petraglia F., Gallinelli A., Cossarizza A., Franceschi C.,
Muscettola M., Genazzani A. D., Surico N. and Genazzani A. R.
(1993) Corticotropin-releasing hormone modulates cytokines
release in cultured human peripheral blood mononuclear cells. Life
Sci. 53, 1735–1742.
Audhya T., Jain R. and Hollander C. S. (1991) Receptor-mediated
immuno-modulation by corticotropin-releasing factor. Cell Immu-
nol. 134, 77–84.
Brunson K. L., Eghbal-Ahmadi M., Bender R., Chen Y. and Baram T. Z.
(2001) Long-term, progressive hippocampal cell loss and dis-
function induced by early-life administration of corticotropin-
releasing hormone reproduce the effects of early-life stress. Proc.
Natl Acad. Sci. USA 98, 8856–8861.
Carlson K. W., Nawy S. T., Wei E. T., Sadee W., Filov V. A., Rezsova
V. V., Sloinski A. and Quillan. J. M. (2001) Inhibition of mouse
melanoma cell proliferation by corticotropin-releasing hormone
and its analogs. Anticancer Res. 21, 1173–1180.
Chen R., Lewis K. A., Perrin M. H. and Vale W. W. (1993) Expression
cloning of a human corticotropin-releasing-factor receptor. Proc.
Natl Acad. Sci. USA 90, 8967–8971.
Chrousos G. P. (1995) The hypothalamic-pituitary-adrenal axis and
immune-mediated inflammation. N. Engl. J. Med. 332, 1351–1362.
Cibelli G., Corsi P., Diana G., Vitiello F. and Thiel G. (2001) Corti-
cotropin-releasing factor triggers neurite outgrowth of a catechol-
aminergic immortalized neuron via cAMP and MAP kinase
signaling pathways. Eur. J. Neurosci. 13, 1339–1348.
Clifton V. L., Owens P. C., Ribinson P. J. and Smith R. (1995)
Identification and characterization of a corticotropin-releasing
hormone receptor in human placenta. Eur. Endocrinol. 133, 591–
597.
De Souza E. B. (1995) Corticotropin-releasing factor receptors: physi-
ology, pharmacology, biochemistry and role in central nervous
system and immune disorders. Psychoneuroendocrinology 20,
789–819.
Dermitzaki E., Tsatsanis C., Gravanis A. and Margioris A. N. (2002)
Corticotropin-releasing hormone onduces Fas ligand production
and apoptosis in PC12 cells via activation of p38 mitogen-activated
protein kinase. J. Biol. Chem. 277, 12280–12287.
Giulian D. (1987) Ameboid microglia as effectors of inflammation in the
central nervous system. J. Neurosci. Res. 18, 155–171.
Greenwood R. S., Zheng F. and Meeker R. (1997) Persistent election
of corticotrophin releasing factor and vasopressin but not oxy-
tocin mRNA in the rat after kindle seizures. Neurosci. Lett. 224,
66–70.
Ha B. K., Bishop G. A., King J. S. and Burry R. W. (2000) Corticotropin
releasing factor induces proliferation of cerebellar astrocytes.
J. Neurosci. Res. 62, 789–798.
Hall-Jackson C. A., Goedert M., Hedge P. and Cohen P. (1999) Effect of
SB203580 on the activity of c-Raf in vitro and in vivo. Oncogene
18, 2047–2054.
Jana M., Dasgupta S., Liu X. and Pahan K. (2002) Regulation of tumor
necrosis factor-a. Expression by CD40 ligation in BV-2 microglial
cells. J. Neurochem. 80, 197–206.
Karalis K., Sano H., Redwine S., Listwak R., Wilder L. and Chrousos
G. P. (1991) Autocrine or paracrine inflammatory actions of corti-
cotropin-releasing hormone in vivo. Science 254, 421–423.
Kostich W. A., Chen A., Sperle K. and Largent B. L. (1998) Molecular
identification and analysis of a novel human corticotropin-releasing
194 W. Wang et al.
� 2003 International Society for Neurochemistry, Journal of Neurochemistry, 84, 189–195
factor (CRF) receptor: the CRF2c receptor. Mol. Endocrinol. 12,
1077–1085.
Kreutzberg G. W. (1996) Microglia: a sensor for pathological events in
the CNS. Trends Neurosci. 19, 312–318.
Lezoualc’h F., Engert S., Berning B. and Behl C. (2000) Corticotropin-
releasing hormone-mediated neuroprotection against oxidative
stress is associated with the increased release of non-amyloido-
genic amyloid beta precursor protein and with the suppression of
nuclear factor-kappaB. Mol. Endocrinol. 14, 147–159.
Li H., Robinson P. J., Kawashima S., Funder J. W. and Liu J. (1998)
Differential regulation of MAP kinase activity by corticotropin-
releasing hormone in normal and neoplastic corticotropes. Int. J.
Biochem. Cell Biol. 30, 1389–1401.
Linthorst A. C., Flachskamm C., Hopkins S. J., Hoadley M. E., Labeur
M. S., Holsboer F. and Reul. J. M. (1997) Long-term intracere-
broventricular infusion of corticotropin-releasing hormone alters
neuroendocrine, neurochemical, autonomic, behavioral, and
cytokine responses to a systemic inflammatory challenge. J. Neu-
rosci. 17, 4448–4460.
Lovenberg T. W., Chen W. L., Grigoriadis D. E., Clevenger W., Chal-
mers D. T., De Souza E. B. and Oltersdorf T. (1995) Cloning and
characterization of a functionally distinct corticotropin-releasing
factor receptor subtype from rat brain. Proc. Natl Acad. Sci. USA
92, 836–840.
Maecker H., Desai A., Dash R., Rivier J., Vale W. and Sapolsky R.
(1997) Astressin, a novel and potent CRF antagonist, is neuro-
protective in the hippocampus when administered after a seizure.
Brain Res. 744, 166–170.
McGillis J. P., Park A., Rubin-Fletter P., Turck C., Dallman M. F.
and Payan D. G. (1989) Stimulation of rat B-lymphocyte
proliferation by corticotropin-releasing factor. J. Neurosci. Res. 23,
346–352.
Merrill J. E. and Jonakait G. M. (1995) Interactions of the nervous
system and immune system development, normal brain home-
ostasis and diseases. FASEB J. 9, 611–618.
Mitsuma T., Matsumoto Y. and Tomita Y. (2001) Corticotropin releasing
hormone stimulates proliferation of keratinocytes. Life Sci. 69,
1991–1998.
Owens M. J. and Nemeroff C. B. (1991) Physiology and pharmacology
of corticotropin- releasing factor. Pharmacol. Rev. 43, 425–473.
Paez Pereda M., Sauer J., Perez Castro C., Finkielman S., Stalla G. K.,
Holsboer F. and Arzt E. (1995) Corticotropin-releasing hormone
differentially modulates the interleukin-1 system according to the
level of monocyte activation by endotoxin. Endocrinology 136,
5504–5510.
Pedersen W. A., McCullers D., Culmsee C., Haughey N. J., Herman J. P.
and Mattson M. P. (2001). Corticotropin-releasing hormone pro-
tects neurons against insults relevant to the pathogenesis of Alz-
heimer’s disease. Neurobiol. Dis. 8, 492–503.
Peletch S. L. and Sanghera J. S. (1992) MAP kinase: charting the reg-
ulatory pathways. Science 257, 1355–1356.
Perrin M., Donaldson C., Chen R., Blount A., Berggren T., Bilezikjian
L., Sawchenko P. and Vale W. W. (1995) Identification of a second
CRF receptor gene and characterization of a cDNA expressed in
heart. Proc. Natl Acad. Sci. USA 92, 2969–2973.
Pyo H., Joe E., Jung S., Lee S. and Jou I. (1999) Gangliosides activate
cultured rat brain microglia. J. Biol. Chem. 274, 34584–34589.
Quevedo M. E., Slominski A., Pinto W., Wei T. and Wortsman J.
(2001) Pleiotropic effects of corticotropin releasing hormone on
normal human skin keratinocytes. In Vitro Cell Dev. Biol. Anim.
37, 50–54.
Robinson M. J. and Cobb M. H. (1997) Mitogen-activated protein kinase
pathways. Curr. Opin. Cell Biol. 9, 180–186.
Roe S. Y., McGowan E. M. and Rothwell N. J. (1998) Evidence for the
involvement of corticotropin-releasing hormone in the pathogene-
sis of traumatic brain injury. Eur. J. Neurosci. 10, 553–559.
Rossant C. J., Pinnock R. D., Hughes J., Hall M. D. and McNulty S.
(1999) Corticotropin-releasing factor type 1 and type 2 alpha
receptors regulate phosphorylation of calcium/cyclic adenosine
3¢,5¢-monophosphate response element-binding protein and acti-
vation of p42/p44 mitogen-activated protein kinase. Endocrinology
140, 1525–1536.
Sapolsky R., Rivier C., Yamamoto G., Plotsky P. and Vale W. (1987)
Interleukin-1 stimulates the secretion of hypothalamic corticotro-
pin-releasing factor. Science 238, 522–524.
Singh V. K. (1989) Stimulatory effect of corticotropin-releasing neuro-
hormone on human lymphocyte proliferation and interleukin-1
receptor expression. J. Neuroimmunol. 23, 257–262.
Singh V. K. and Leu S. J. (1990) Enhancing effect of corticotropin-
releasing neurohormone on the production of interleukin-1 and
interleukin-2. Neurosci. Lett. 120, 151–154.
Singh V. K. and Fudenberg H. H. (1988) Binding of [125I]corticotropin
releasing factor in blood immunocytes and its reduction in Alz-
heimer’s disease. Immunol. Lett. 18, 5–8.
Strijbos P. J. L. M., Relton J. K. and Rothwell N. J. (1994) Corticotropin-
releasing factor antagonist inhibits neuronal damage induced by
focal cerebral ischaemia or activation of NMDA receptors in the rat
brain. Brain Res. 656, 405–408.
Tournier C., Pomerance M., Gavaret J.-M. and Pierre M. (1994) MAP
kinase cascade in astrocytes. Glia 10, 81–88.
Vale W., Spiess J., Rivier C. and Rivier J. (1981) Characterization of a
41-residue ovine hypothalamic peptide that stimulates secretion of
corticotropin and b-endorphin. Science 213, 1394–1397.
Vamvakopoulos N. C. and Chrousos G. P. (1994) Hormone regulation of
human corticotropin-releasing hormone gene expression: implica-
tions for the stress response and imune/inflammatory reaction.
Endocr. Rev. 15, 409–420.
Wang W., Ross G. M., Riopelle R. J. and Dow K. E. (2000) Sublethal
hypoxia up-regulates corticotropin releasing factor receptor type 1
in fetal hippocampal neurons. Neuroreport. 11, 3123–3126.
Wang W., Ji P., Riopelle R. J. and Dow K. E. (2002) Functional
expression of corticotropin-releasing hormone receptor 1 in cul-
tured rat microglia. J. Neurochem. 80, 287–294.
Wong M. L., Loddick S. A., Bongiorno P. B., Gold P. W., Rothwell N. J.
and Licinio J. (1995) Focal cerebral ischemia induces CRH mRNA
in rat cerebral cortex and amygdala. Neuroreport 11, 1785–1788.
CRH induces TNF-a release in microglia 195
� 2003 International Society for Neurochemistry, Journal of Neurochemistry, 84, 189–195







![[PPT]PowerPoint Presentation - ITU: Committed to … · Web viewLightning flashes provide a high current (hundreds kA) in a very short time (μs), releasing a very high power in the](https://static.fdocument.org/doc/165x107/5ad34fd37f8b9a482c8d7dce/pptpowerpoint-presentation-itu-committed-to-viewlightning-flashes-provide.jpg)











![Epac2 signaling at the β-cell plasma membrane920771/FULLTEXT01.pdf · small fraction of cells are pancreatic polypeptide-secreting PP-cells [6] and ghrelin-releasing ε-cells [7].](https://static.fdocument.org/doc/165x107/6065b034c80f1b4fbb7d2949/epac2-signaling-at-the-cell-plasma-membrane-920771fulltext01pdf-small-fraction.jpg)





