The low viral production in trophoblastic cells is due to a high ...
Transcript of The low viral production in trophoblastic cells is due to a high ...

The low viral production in trophoblastic cells
is due to a high endocytic internalization of the human immunodefiency virus type 1
and can be overcome by the pro-inflammatory cytokines TNF-α and IL-1
Gaël Vidricaire, Mélanie R. Tardif and Michel J. Tremblay*
Centre de Recherche en Infectiologie, Hôpital CHUL, Centre Hospitalier Universitaire de
Québec, and Département de Biologie médicale, Faculté de Médecine,
Université Laval, Ste-Foy, Québec, Canada, G1V 4G2
*Corresponding author. Mailing address:
Laboratoire d'Immuno-Rétrovirologie Humaine
Centre de Recherche en Infectiologie, RC709
Hôpital CHUL, Centre Hospitalier Universitaire de Québec
2705 boul. Laurier
Ste-Foy,Québec, Canada, G1V 4G2
Phone: (418) 654-2705; Fax: (418) 654-2212
E-mail: [email protected]
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

2
ABSTRACT
Maternal-infant transmission of human immunodeficiency virus type-1 (HIV-1) is the primary
cause of this retrovirus infection in neonates. Although the mechanism(s) through which HIV-1
crosses the placenta to reach the fetus remains unclear, trophoblasts have been proposed to play a
critical role in modulating virus spread to the fetus. Thus, this paper addresses the mechanism of
HIV-1 biology in trophoblastic cells. The trophoblastic cell lines BeWo, JAR and JEG-3 were
infected with reporter HIV-1 particles pseudotyped with envelope glycoproteins from the
vesicular stomatitis virus or various strains of HIV-1. We demonstrate that despite a high
internalization process of HIV-1 and no block in viral production, HIV-1 established a limited
infection of trophoblasts with the production of very few progeny viruses. The factor responsible
for this restriction to virus replication in such a cellular microenvironment is that the intracellular
p24 is concentrated predominantly in endosomal vesicles following HIV-1 entry. Interestingly,
HIV-1 transcription and virus production of infectious particles were both augmented upon
treatment of trophoblasts with TNF-α and IL-1. However, the amount of progeny virions released
by trophoblasts infected with native HIV-1 virions was so low even in the presence of pro-
inflammatory cytokines that a co-culture step with indicator cells was necessary to detect virus
production. Collectively these data illustrate for the first time that the natural low permissiveness
of trophoblasts to productive HIV-1 infection is due to a restriction in the mode of entry and such
a limitation can be overcome with physiologic doses of TNF-α and IL-1, which are both
expressed by the placenta, in conjunction with cell-cell contact. Considering that there is a linear
correlation between viral load and HIV-1 vertical transmission, the environmental milieu may
thus contribute to the propagation of HIV-1 across the placenta.
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

3
INTRODUCTION
Mother-to-child transmission of the human immunodeficiency virus type 1 (HIV-1) is a
serious public health issue. An estimated 2.4 million infected women give birth annually and
1,600 infants acquire HIV-1 infection every day worldwide (reviewed in (1)). In the absence of
antiretroviral treatment, the reported risk of vertical transmission lies within the range of 10 to
39% (1-3). Vertical transmission of HIV-1 from mother-to-child can occur prepartum (in utero
involving transplacental passage) and intrapartum (at birth upon exposure of the infants’ skin and
mucous membrane to maternal blood and vaginal secretion) (4-6). Mathematical modeling has
allowed estimating that 30% of infections occur in utero less than two months before birth and
65% at birth (7). Transmission of HIV-1 during early gestation also occurs since HIV-1 has been
detected in 8-week aborted foetuses and in second trimester fetal tissues (8-11).
In order for the virus to reach the fetal circulation and infect the foetus in utero, HIV-1 must
cross the placental barrier which is made of a double layer of polarized epithelial-type cells, the
cytotrophoblasts and syncytiophoblasts. These cells separate the maternal and fetal blood
circulations and control fluxes between the two circulations. Several published reports have
addressed the question as to how HIV-1 reaches the foetus. It has been shown that the placenta
may allow transcytosis of the virus from the maternal to the foetal circulation (12). Alternatively
and/or concomitantly, the virus may infect the placenta to reach the fetal circulation and
ultimately the foetus. Indeed, HIV-1 has been detected on both the maternal and foetal portions of
the placenta, i.e. in decidual macrophages, leukocytes, trophoblasts, Hofbauer cells, in villous
endothelial cells and CD3-expressing placental cells (8, 13-18). Moreover, some authors have
shown that HIV-1 undergoes productive replication in the placenta. The analysis of the
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

4
evolutionary relationships of HIV-1’s sequences clearly linked maternal sequences with
associated sequences in the trophoblasts and put them on distinctive branches (3). In addition,
human choriocarcinoma cell lines (i.e. BeWo, JAR and JEG-3) as well as isolated primary
trophoblastic cells (including cytotrophoblasts from term placenta and cytotrophoblasts from term
placenta induced to differentiate in syncytiotrophoblasts in vitro) and Hofbauer cells were shown
to be weakly permissive to HIV-1 infection in vitro and to sustain low level of virus replication.
However, other scientists have failed to detect the presence of HIV-1 in the placenta of infected
mothers and/or replication of the virus in these cells (19). Thus, it remains controversial whether
HIV-1 can sustain a productive cycle in trophoblastic cells, but if indeed possible, it is clear that it
is magnitudes lower than in CD4-positive T lymphocytes. The reasons behind this limited
infection are ill defined but are thought to be due to factors related to HIV-1’s phenotype in
conjunction with particular cellular environments. This may include limitations in virus entry,
intra-cellular restriction, inappropriate cellular environment or a combination of the three
(reviewed in (20)). The question of viral entry is crucial since the expression of HIV-1’s cellular
receptor CD4 is very low whereas the expression of HIV-1’s co-receptors, CXCR4 and CCR5,
may decline from the first to third trimester of gestation. This may account for a limited viral
entry (9, 21-24). However, the process of viral entry per se in trophoblastic cells has not been
investigated thus far.
A key feature of pregnancy is the production of a vast array of cytokines (e.g. IL-1, IL-3, IL-4,
IL-6, IL-10, GM-CSF, M-CSF, LIF, TGF-β, IFN-γ and TNF-α), hormones, growth factors (e.g.
EGF, VEGF, progesterone and oestrogen) and prostaglandins (e.g. PGE2) in a developmentally
regulated fashion by the conceptus and/or the uterus. These agents play pivotal roles during
gestation and are mandatory for a successful pregnancy (reviewed in (25-27)). On the other hand,
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

5
some of these agents are also known to be up-regulated in vivo in HIV-1-infected patients and to
modulate viral expression in vitro (reviewed in (20, 28)). We previously tested the ability of
factors known to be present in the vicinity of the trophoblast during gestation and for which
trophoblastic cells express the appropriate receptors to drive HIV-1 transcriptional activity in
trophoblats. Among all the soluble agents tested (i.e. EGF, GM-CSF, IFN-γ, IL-1α, IL-1β, IL-3,
IL-4, IL-6, IL-7, IL-8, IL-10 IL-12, LIF, M-CSF, NGF, PGE2, TGF-β and TNF-α), only two
cytokines, TNF-α and IL-1, were found to strongly activate virus transcription (29). Thus,
specific cytokines and/or modulatory factors present in the placental microenvironment while
controlling cellular activities may also play a regulatory role in protecting the host or, inversely,
in driving HIV-1 expression. More specifically, since HIV-1 may be present in too low
concentration and/or may be latent, some of these factors could be, in part, the triggering element
necessary for the expression of HIV-1 in infected trophoblastic cells. This would translate into
productive viral expression and spreading of the virus to the foetus.
The central objective of the present work was to provide further insight on the susceptibility of
human trophoblast to a productive infection with HIV-1. To this end, we conducted experiments
with both fully infectious HIV-1 particles and recombinant HIV-1-based reporter viruses
pseudotyped with the envelope proteins of the broad-host-range vesicular stomatitis virus (VSV-
G) and certain strains of HIV-1. The pseudotyping strategy with VSV-G allows bypassing the
natural mode of HIV-1 entry and not only broadens the natural virus tropism but also
significantly enhances virus infectivity (30). Contrary to previous assumptions, we demonstrate
for the first time that the reason for the limited HIV-1 infection of trophoblastic cells is not linked
with ineffective virus internalization since we found massive HIV-1 entry in trophoblastic cells.
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

6
Rather, the subcellular distribution of viral p24 was predominantly located in the vesicular
fraction, an event accounting for the weak virus production in such cells. On the other hand, we
showed that trophoblastic cells possess no block in viral transcription or viral production. We
showed that TNF-α and IL-1 triggered an important increase in viral gene expression. However,
production of progeny virions upon treatment with these pro-inflammatory cytokines was only
seen following co-cultivation with susceptible indicator cells. These data represent further
evidence that the natural low permissiveness of trophoblasts to productive HIV-1 infection is
associated with limitations in the early events of the virus life cycle. Our results suggest that the
presence of cytokines such as TNF-α and IL-1 in the vicinity of trophoblastic cells in association
with lymphocytic cells would create favorable conditions leading to vertical transmission of this
retrovirus. Considering that expression of these cytokines is highly regulated according to the
stage of placental development, it can be proposed that windows of opportunity are transiently
created for the induction of viral expression by extracellular factors in trophoblasts. Collectively,
the data presented may explain in part the mechanism of HIV-1’s transmission to the foetus
during gestation.
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

7
MATERIALS AND METHODS
Cells. The malignantly transformed human cell lines of trophoblast lineage BeWo, JAR and JEG-
3 were obtained from the American Tissue Culture Collection (Manassas, VA). The human
embryonic kidney cell line 293T (expressing the simian virus 40 large T antigen) was kindly
provided by W. C. Greene (J. Gladstone Institutes, San Francisco, Ca). The JAR, JEG-3 and
293T cells lines were cultured in DMEM medium (Gibco-BRL, Burlington, Canada) whereas the
BeWo cell line was maintained in F12 Nutrient Mixture (Gibco-BRL, Burlington, Canada). Both
media were supplemented with 10% fetal bovine serum (FBS) (Invitrogen Life Technologies,
Burlington, Canada), glutamine (2 mM), penicillin G (100 U/ml) and streptomycin (100 mg/ml).
BeWo, JAR and JEG-3 cells were routinely subcultured at a seeding density of 3 x 106 cells and
293T cells at 1 x 106 cells in 75 cm2 tissue culture flasks. PM1 cells were obtained through the
AIDS Research and Reference Reagent Program (Division of AIDS, National Institute of Allergy
and Infectious Diseases, Rockville, MD). These cells were cultured in RPMI 1640 medium
supplemented with 10% FBS. The reporter LuSIV cell line, kindly provided by J. E. Clements
(Johns Hopkins University School of Medicine, Baltimore, MD), was derived from the CEMx174
parental cell line (B-cell / T-cell hybrid) and carries the luciferase reporter gene under the control
of the SIVmac239 LTR. These cells were maintained at 0.5 x 106 cells/ml in selection medium
made of RPMI 1640 (Gibco-BRL, Burlington, Canada) with 10% FBS, 15 mM NAOH, 25 mM
HEPES, and supplemented with glutamine (2 mM), penicillin G (100 U/ml), streptomycin (100
mg/ml) and 300 µg/ml hygromycin B (Boehringer Ingelheim, Indianapolis, IN). Human
peripheral blood mononuclear cells (PBMCs) from healthy donors were isolated by centrifugation
through a Ficoll-Hypaque density gradient. PBMCs were resuspended at a density of 106 cells/ml
in RPMI 1640 with 20% FBS, 15 mM NAOH, 25 mM HEPES and supplemented with glutamine
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

8
(2 mM), penicillin G (100 U/mL), streptomycin (100 mg/ml), 3 µg/ml of PHA-P (Sigma, St-
Louis, Mo) and 50 U/ml of human recombinant IL-2 (kind gift of M. Gately, Hoffman-Laroche
Inc.) (31).
Molecular constructs. pNL4-3 is a full-length infectious molecular clone of HIV-1 while the
NL4-3-Luc E-R+ vector was constructed by inserting a frame shift mutation near the env gene and
the firefly luciferase reporter gene into the nef gene (32, 33). Both molecular constructs were
obtained through the AIDS Repository Reagent Program. The pHCMV-G molecular construct
codes for the broad-host-range vesicular stomatitis virus envelope glycoprotein G (VSV-G) under
the control of the human cytomegalovirus promoter (34). The pcDNA-1/Amp-based expression
vector coding for the HIV-1 Ada-M (M-tropic) full-length envelope protein was generously
provided by N. R. Landau (The Salk Institute for Biological Studies, La Jolla, CA). pHXB2-env
is a mammalian expression vector coding for the HIV-1 HXB2 (T-tropic) envelope glycoprotein
and was obtained from the AIDS Repository Reagent Program. pLTR-Luc and pmκBLTR-Luc
have been kindly provided by Dr. K. Calame (Columbia University, New York, NY). These
molecular constructs contain the luciferase reporter gene under the control of wild-type
(GGGACTTTCC) or NF-κB-mutated (CTCACTTTCC) HIV-1HXB2 LTR (453 to +80) (35). The
molecular construct pNF-κB-Luc contains five (5) consensus sequences of NF-κB binding sites
placed in front of the luciferase reporter gene (Stratagene, La Jolla, CA). The reporter gene
vectors pBlue3’LTR-Luc-A to G carry the HIV-1 LTR regions from subtype A, B, C, D, E, F,
and G driving the firefly luciferase reporter gene (obtained through the AIDS Repository Reagent
Program) (36).
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

9
Preparation of virus stocks. Viruses were produced by calcium phosphate transfection of
293T cells, as described previously (37, 38). Briefly, 293T cells were plated 16 h before
transfection to reach a 50 to 80% confluence the day of transfection. Using the Clontech
Transfection Kit (BD Biosciences Clonetech, Palo Alto, CA), cells were co-transfected with
NL4-3-Luc E-R+ along with a vector coding for VSV-G, Ada-M-env, or HXB2-env to produce the
luciferase expressing single-cycle pseudotyped HIV-1 virions. Fully infectious viral entities were
produced by transiently transfecting 293T cells with the infectious molecular clone pNL4-3 or by
co-transfection with pNL4-3 and pHCMV-G. Sixteen hours after transfection, the cells were
washed twice with phosphate-buffered saline (PBS) and incubated for 24 h in complete DMEM
culture medium. Pseudotypes and fully infectious viruses were collected at this point by filtering
the culture media through a 0.22 µM pore size cellulose acetate membrane (Millipore, Bedford,
MA). Virus stocks were aliquoted and frozen at -85°C for future use. All virus preparations
underwent only one freeze-thaw cycle before initiation of infection studies. Virus stocks were
normalized for virion content by using a p24 antibody capture assay developed in our laboratory
(39).
Virus entry and cell fractionation assays. Approximately 1 x 106 of JAR and PM1 cells were
incubated with Aad-M or VSV-G pseudotyped HIV-1 particles (200 ng of p24) in 6-well tissue
culture plates at 37˚C for a period of 5 min to 4 h. Cells were next extensively washed with ice-
cold PBS and trypsinized for 5 min at 37˚C. The cells were then washed with RPMI
supplemented with 10% FBS followed by three washes with ice-cold PBS. For cell entry assays,
cells were resuspended in lysis buffer (20 mM HEPES [pH 7,4], 150 mM NaCl, 0,5% Triton X-
100). The level of p24 was determined by an in-house enzymatic assay as previously described
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

10
(39). For cell fractionation assays, to disrupt cellular membranes, cells were resuspended in 1 ml
of ice-cold hypotonic buffer (10 mM Tris-HCl [pH 7.5], 10 mM KCl, 1 mM EDTA) for 1 min
and broken by Dounce homogenization (three strokes, 7 ml B pestles). Nuclei, cell debris and
undamaged cells were pelleted by centrifugation (1,800 rpm for 5 min at 4˚C). Supernatants
containing cytosol and vesicles (including endosomes) were centrifuged at 12,000 rpm for 90 min
at 4˚C in a Heraeus centrifuge. Supernatant that represents the cytosolic fraction was adjusted to
0.5% Triton X-100 while the pellet which is the vesicular fraction was resuspended in 1 ml of
lysis buffer (20 mM HEPES [pH 7,4], 150 mM NaCl, 0,5% Triton X-100). The level of p24
present in each fraction was assessed using the p24 assay (39).
Virus infection, luciferase assays and co-culture experiments. In 25 or 75 cm2 tissue
culture flasks, 2 to 6 x 106 BeWo, JAR, or JEG-3 cells were incubated at 37ºC under a 5% CO2
atmosphere for 7 h with luciferase-encoding HIV-1 particles pseudotyped with VSV-G (6 to 145
ng of p24), Ada-M, or HXB2 envelope glycoproteins (250 to 400 ng of p24). Cells were then
washed three times with PBS, trypsinized and subcultured at 25 x 103 cells per well in 96-well
flat-bottom tissue culture plates or at 50 x 103 cells per well in 48-well flat-bottom tissue culture
plates in 200 µl of complete DMEM culture medium. After an overnight incubation, 100 µl of
medium was removed from each well and replaced with 100 µl of culture medium supplemented
with the following agents: tumor necrosis factor (TNF)-α (R&D Systems, Minneapolis, MN),
interleukin (IL)-1α or IL-1β (National Cancer Institute, Rockville, MD). After an 8 to 72 h
incubation period, luciferase activity was monitored in cell lysates as previously described (40).
For co-culture experiments, 1 x 106 JAR cells were incubated in 25 cm2 tissue culture dishes at
37ºC for 7 h with fully competent NL4-3 particles (400 ng of p24). Cells were then washed three
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

11
times with PBS, trypsinized and subcultured at 1 x 105 cells per well in 12-well flat-bottom tissue
culture plates in 1.3 ml of complete DMEM culture medium. After an overnight incubation, 650
µl of culture medium was removed from each well and replaced with 650 µl of fresh complete
DMEM culture medium supplemented with TNF-α at a final concentration of 10 ng/ml. After a
24 h stimulation period, the infected JAR cells were co-cultured for 24 h with 4 x 105 indicator
cells (i.e. LuSIV or PBMCs). Indicator cells that remained in suspension were removed from the
attached JAR cells, centrifuged for 5 min at 1,200 RPM and resuspended in the appropriate
culture medium. The rescued LuSIV and PBMCs were seeded in 48-well plates at 3 x 105 cells
per well. On each subsequent day, 100 µl of LuSIV or 150 µl of cell-free culture media from the
PBMCs were transferred to 96-well plates and lysed. The lysed cells and culture media were
frozen. Finally, luciferase activity and p24 level were assessed in lysed LuSIV and in PBMCs
culture media, respectively.
Transient transfection of JAR cells. JAR cells were transiently transfected by calcium
phosphate precipitation using the Clontech Transfection Kit. Briefly, 0.5 to 1.5 x 106 JAR cells
were plated 16 h before transfection in 25 cm2 tissue culture dishes. For each transfection, 5 µg of
plasmid DNA were used. For the HIV-1 Clades A to G transfection experiment, JAR cells were
co-transfected with 1 µg of an actin promoter-driven β-galactosidase vector (pActin-β-
galactosidase) to normalize for transfection efficiency. Sixteen h after transfection, the cells were
washed twice with PBS and incubated for 8 h in complete DMEM culture medium. The
transfected cells were then washed three times with PBS, trypsinized and subcultured at 25 x 103
cells per well in 96-well flat-bottom tissue culture plates or at 50 x 103 cells per well in 48-well
flat-bottom tissue culture plates in 200 µl of complete DMEM culture medium. After an
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

12
overnight incubation, 100 µl of medium was removed from each well and replaced with 100 µl of
fresh complete DMEM culture medium supplemented with TNF-α at a final concentration of 10
ng/ml. After a 8 h stimulation period, 100 µl of cell-free culture media were removed and 25 µl
of a 5X luciferase assay lysis buffer were added. Luciferase activity was measured as described
above. β-galactosidase assays were performed using the Galacto Light™ chemiluminescent
reporter assay for β-galactosidase (Tropix, Bedford, MA).
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

13
RESULTS
Early events in the HIV-1 replicative cycle represent rate-limiting steps for virus infection of
trophoblast-derived malignant cell lines. Given the reported low susceptibility of trophoblastic
cells to productive HIV-1 infection (22, 23, 41), we initially defined the permissiveness of
malignantly transformed cell lines of trophoblast lineage to the early events in HIV-1 biology.
This goal was reached by inoculating BeWo, JAR and JEG-3 with luciferase expressing single-
cycle HIV-1 particles pseudotyped either with the envelope protein of HXB2 (T-tropic HIV-1
strain), Ada-M (macrophage-tropic HIV-1 strain), or the envelope G protein of VSV (i.e. VSV-
G). A previous study has shown that pseudotyping of HIV-1 particles with VSV-G results in both
a marked enhancement of virus infectivity and in an extended cellular tropism (30). Exposure of
BeWo, JAR and JEG-3 cell lines to HXB2 and Ada-M pseudotypes yielded a very low
spontaneous HIV-1 LTR-directed reporter gene activity (Table 1). However, when these cells
were exposed to single-cycle VSV-G pseudotyped reporter viruses, a significant enhancement in
luciferase activity was observed. The highest augmentation in HIV-1 transcriptional activity was
obtained for JAR and the lowest for BeWo. Based on these observations, it can be concluded that
the failure of HIV-1 to productively infect human trophoblast cells is related with a blockade in
the early steps in the virus life cycle.
Virus internalization shows no restriction in trophoblastic cells. We next verified whether the
limitation in HIV-1 production was at the level of internalization since trophoblastic cells are
reported to express either no or very little CD4 and CXCR4 or CCR5. JAR cells were exposed to
VSV-G pseudotypes, Ada-M pseudotypes or fully infectious NL4-3 for 5 min to 4 h at 370C.
Subsequently, the cells were trypsinized, washed and lysed before monitoring the amount of
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

14
internalized virus. We found that the three virus preparations tested were able to enter with high
efficiency and in a timely fashion in the trophoblastic cell line JAR (Fig. 1). Surprisingly enough,
VSV-G and Ada-M pseudotypes were found to enter JAR cells at a comparable level, therefore
suggesting that the blockade in HIV-1 transcriptional activity in trophoblast cells is not associated
with a barrier that limits the process of HIV-1 attachment and internalization.
HIV-1 is found predominantly in the vesicular fraction upon viral entry into trophoblastic
cells. In order to define the exact location of HIV-1 upon virus entry into trophoblasts, JAR cells
were exposed to Ada-M pseudotyped HIV-1 particles for a short period of time and we measured
the amount of viruses present in the cytosolic and vesicular fractions. A similar technical
approach was used with PM1 cells, a CD4-expressing T lymphoid cell line known to be highly
susceptible to HIV-1 infection. Although we observed comparable absolute amounts of
intracellular p24 levels in JAR and PM1 cells, differences were detected with respect to
intracellular p24 in cytosolic and vesicular fractions. In JAR cells, at 30 min following virus
exposure, Ada-M pseudotyped viruses were present in the vesicular fraction only (Fig. 2A).
Vesicular and cytosolic p24 represented 82% and 18%, respectively, of total intracellular p24
after 2 h of virus exposure. The distribution of intracellular p24 between the cytosolic and
vesicular fractions was different in PM1 cells. For example, after 2 h of exposure to Ada-M
pseudotypes, vesicular and cytosolic p24 in PM1 cells represented 65% and 35%, respectively, of
the total intracellular p24 (Fig. 2B). Our findings indicate that HIV-1 internalization in
trophoblastic cells is a highly efficient process but the route of entry is mediated in large part
through endosomal vesicles. Given that productive HIV-1 infection has been proposed to result
from the cytosolic release of p24 (42), the reduced susceptibility of trophoblast to HIV-1
infection is due to an extensive vesicular uptake.
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

15
HIV-1 LTR-driven reporter gene activity is increased in trophoblastic cells by TNF-α, IL-1α
and IL-1β. Based on our present data, we now know that HIV-1 is indeed present in the
cytoplasm of trophoblastic cells, albeit at a low concentration. We therefore argue that these
viruses can lead to a productive infection. This notion is controversial since other scientists have
failed to detect HIV-1’s replication in trophoblastic cells. Two hypotheses can be made: 1) either
the virus is integrated and becomes latent and/or 2) the virus is present in such a low
concentration in the cytoplasm that viral expression resulting from these viruses may be too low
to be detected. In both instances, external stimulus may be required to detect viral gene
expression. Numerous extra-cellular soluble factors are present in the vicinity of the placenta
during gestation and some of them are known to modulate HIV-1’s expression in other cellular
environment. We tested the effect of TNF-α, IL-1α and IL-1β to trigger the viral regulatory
elements in trophoblastic cells by using recombinant luciferase-expressing HIV-1 pseudotyped
with envelope glycoproteins from Ada-M or HXB2 strain of HIV-1. In agreement with our
previous findings, no increase in luciferase activity could be detected in untreated JAR cells
following infection with Ada-M or HXB2 pseudotypes. However, a significant enhancement of
HIV-1 LTR activity was observed upon exposure of such virally infected JAR cells to TNF-α and
IL-1β (Fig. 3). For example, incubation of Ada-M-infected JAR cells with increasing doses of
TNF-α and IL-1β led to a maximal 87.3 and 26.3-fold increase in LTR activity, respectively. A
similar treatment of JAR cells once infected with HXB2 pseudotypes resulted also in induction of
HIV-1 LTR-dependent reporter gene activity but to a smaller extent. Similar observations were
made when JAR cells were treated instead with IL-1α (data not shown). Further studies revealed
that the positive effect of TNF-α, IL-1α and IL-1β on virus transcriptional activity was dose
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

16
dependent (Fig. 4). To demonstrate that the noticed effect was not cell type-specific, we tested the
effect of TNF-α, IL-1α and IL-1β on two other trophoblastic cell lines, i.e. BeWo and JEG-3.
Following virus infection, HIV-1 LTR-driven luciferase expression was enhanced in a dose-
dependent manner by the three tested cytokines in BeWo cells (Fig. 5). The highest levels of
reporter gene activity were seen following treatment of BeWo cells with TNF-α (i.e. 8.2-fold
increase with the highest dose of TNF-α. Exposure of BeWo cells to IL-1α and IL-1β produced a
4-fold increase in HIV-1 LTR activity. Similar data were obtained when using JEG-3 cells (data
not shown).
Production of fully infectious HIV-1 particles by trophoblastic cells is only seen following
treatment with TNF-α and co-culture with indicator cells. In order to investigate whether the
cytokine-mediated up-regulation of HIV-1 transcriptional activity could be seen in the context of
the complete viral genome, JAR cells were inoculated with fully infectious HIV-1NL4-3 viruses
before exposure to TNF-α. Virus production was found to be near the detection limit of our p24
enzymatic assay (i.e. less than 50 pg/ml) despite exposure to TNF-α (data not shown). We next
attempted to rescue the seemingly low amount of produced viruses by co-cultivation with the
CXCR4-expressing LuSIV cell line. Previous experiments performed in our laboratory suggest
that such indicator cells are susceptible to infection with very low levels of HIV-1, i.e. less than 1
pg of p24 (unpublished observations). No noticeable increase in luciferase activity was obtained
in LuSIV co-cultured with virus-infected JAR cells that were left unstimulated (Fig. 6A).
However, the co-cultivation of LuSIV cells with TNF-α-treated JAR cells that were initially
infected with NL4-3 resulted in a dramatic augmentation of luciferase activity. To more closely
parallel physiological conditions, similar studies were carried out using PBMCs as indicator cells.
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

17
When PBMCs were co-cultured with unstimulated virus-infected JAR cells, virus production was
again below the detection limit of our p24 assay (Fig. 6B). Interestingly, virus production was
rescued when PBMCs were instead co-cultured with NL4-3-infected JAR cells that were also
treated with TNF-α. Again, these data fully support the notion that human trophoblast cells
produced only low amounts of mature virus progeny, levels that can be significantly augmented
upon treatment with a pro-inflammatory cytokine such as TNF-α.
The major limiting step of HIV-1 infection in trophoblasts is at the level of the route of entry
and is not related to intracellular restrictions. The natural low susceptibility of trophoblast cells
to be productively infected with HIV-1 could be due, in addition to the demonstrated significant
vesicular uptake, to some undefined intracellular restrictions to virus replication. To shed light on
this issue, JAR cells were infected with fully competent HIV-1NL4-3 viruses that bear also the
VSV-G envelope glycoproteins before exposure to TNF-α. This technical strategy permits to
bypass the natural inefficient route of HIV-1 entry in trophoblasts and ultimately to the release of
complete HIV-1 particles. In JAR cells infected with complete NL4-3 virions pseudotyped with
VSV-G envelope glycoproteins, the release of a significant amount of p24 was detected
throughout the course of infection and virus production was again markedly augmented by a
treatment with TNF-α (Fig. 7). Thus no intracellular restriction is present in trophoblatic cells and
together these studies suggest that the route of HIV-1 entry is the major limiting step of HIV-1
infection in trophoblasts.
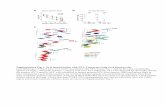
Different HIV-1 LTR subtypes are transactivated by TNF-α and IL-1β in trophoblasts. To
assess whether changes in the LTR architecture due to the recognized genetic heterogeneity of
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

18
HIV-1 can influence the cytokine-mediated modulatory effect seen in trophoblast cell lines,
transfection experiments were conducted with molecular constructs made of various LTR
subtypes. JAR cells were transiently transfected with luciferase-encoding vectors carrying LTR
region from clades A through G before treatment with TNF-α and IL-1β. As shown in Fig. 8,
virus transcription was triggered by both TNF-α and IL-1β for all the HIV-1 LTR clades tested.
This indicates that the up-regulating effect of these cytokines on HIV-1 transcription is not
restricted to a specific HIV-1 LTR subtype.
Cytokine-dependent up-regulation of HIV-1 LTR activity in trophoblasts is mediated via NF-
κB. Finally, we investigated the molecular events leading to TNF-α-induced transactivation of
HIV-1 by transiently transfecting the JAR cell line with various expression vectors before
exposure to TNF-α. As depicted in Fig. 9, TNF-α triggered a 4.4-fold increase in luciferase
activity in JAR cells transfected with the luciferase reporter gene placed under the control of
wild-type HIV-1HXB2 LTR when compared to untreated JAR cells. However, this induction was
lost when JAR cells were transfected with a vector that bears mutations at the two NF-κB-binding
sites within the HIV-1HXB2 LTR domain. The involvement of NF-κB in this process was
confirmed by the observation that a 7.4-fold increase in luciferase activity was obtained upon the
addition of TNF-α to JAR cells that were transfected with a κB-driven reporter gene vector.
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

19
DISCUSSION
The overall objectives of the present study was to provide additional information on the
possible mechanism(s) responsible for the weak susceptibility of trophoblastic cells to productive
HIV-1 infection and to define if cytokines present in the environmental milieu surrounding HIV-
1-infected trophoblasts could positively modulate virus expression. In the present report, a strong
spontaneous activation of the HIV-1 LTR domain was seen in the three choriocarcinoma cell
lines tested (BeWo, JAR and JEG-3) following infection with HIV-1 particles pseudotyped with
VSV-G. This set of data clearly indicates that virus transcription is highly efficient in
trophoblastic cells. These results are in agreement with a previous work that showed that
choriocarcinoma cell lines support basal and Tat-transactivated transcriptional activity of HIV-1
reporter gene constructs (17). However, a minimal HIV-1 LTR-mediated reporter gene activity
was detected when infection of trophoblastic cells was allowed to proceed with viruses bearing
macrophage-tropic and T-tropic HIV-1 envelope glycoproteins. This series of investigations
suggest that the most proximal events in HIV-1 biology represent major limiting steps of virus
infection in trophoblasts.
It has been proposed that the reason behind the limited HIV-1 infection of trophoblastic cells
is due to a block at virus entry, which could be caused by a minimal expression of CD4 and
appropriate chemokine co-receptor (21-24). In the present study, contrary to what was assumed,
we provide evidence that HIV-1 enters massively into trophoblastic cells. Subcellular
fractionation techniques that segregate between vesicular and cytosolic fractions revealed that a
major part of intracellular p24 is found in endosomal vesicles, implying thus that HIV-1 enters
trophoblastic cells predominantly via endocytosis. This route of entry reveals important
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

20
consequence for the virus life cycle in trophoblastic cells. Indeed, recent findings have shown that
HIV-1 entry can occur through plasma membrane fusion and endocytosis in both HeLA and
Jurkat cells. The latter mode of entry usually leads to a nonproductive process of infection since
viruses will ultimately be degraded in lysosomes (43). In trophoblastic cells, phagocytosis is
thought to play an important role in the extensive tissue remodelling that occurs during
trophoblastic invasion of the deciduas and in the control of exchanges between the maternal and
foetal circulations. Moreover, trophoblastic cells actively transcytose several molecules including
immunoglobulins and even pathogens such as HIV- 1 (12). Thus, based on our findings and the
current literature, it is likely that a fraction of HIV-1 entering trophoblasts is transcytosed and
another part is trapped in endocytic vesicles and ultimately degraded. The sum of these two
mechanisms would account for the low permissiveness of trophoblasts to productive HIV-1
infection.
The pro-inflammatory cytokines TNF-α, IL-1α and IL-1β were found to act as potent inducers
of HIV-1 LTR-dependent activity in trophoblasts when these cells were infected with VSV-G
pseudotypes. Interestingly, the same cytokines also induced viral transcription in trophoblastic
cells exposed to replication-defective reporter viruses bearing HIV-1 Ada-M or HXB2 envelope
glycoproteins. These findings are supported by a recent study showing that HIV-1 LTR activity is
increased by TNF-α and IL-1β in primary isolated human trophoblast cells that were transiently
transfected with an HIV-1-based reporter vector (44). Data from this study were entirely based on
transient transfection of HIV-1 LTR-based reporter constructs in trophoblast cells. In contrast,
our observations are founded on integrated proviruses, i.e. following infection of trophoblasts
with either complete HIV-1 particles or HIV-1-based pseudotyped viruses. This is important to
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

21
note since recent findings indicate that integrated proviral DNA behaves quite differently from
transfected plasmids. Indeed, expression of integrated human retroviruses such as HIV-1 and
HTLV-1 has been shown to require cellular factor different from those necessary for expression
of transiently transfected retroviral-based plasmids (45-48). More specifically, it has been
demonstrated that transcription from integrated versus transiently introduced retroviral LTRs
does not proceed via identical signal transduction pathways. This suggests that the signaling
requirements necessary to achieve expression of an integrated proviral DNA can differ from a
transfected viral plasmid. Since the process of integration into the host chromosome is an
obligatory step in HIV-1 life cycle, the series of investigations that we performed with integrated
HIV-1 provide physiological significance to our work.
Concerning possible restrictions at late events in the HIV-1 life cycle, we found that
trophoblast cells sustained high virus production when infection was performed with VSV-G
pseudotypes HIV-1-based viruses. Thus, it can be concluded that, apart from an inefficient route
of virus entry, there is no blockade at late steps in the replicative cycle of HIV-1 in trophoblast.
The minor fraction of intracellular p24 that is found in trophoblast is not sufficient to lead to a
measurable virus production since a co-culture step with indicator cells is necessary to detect
virus production. Under in vivo situations, trophoblasts are in close contact with cells such as
lymphocytes that show a higher susceptibility to HIV-1 entry and productive infection. Thus, it
can be proposed that in spite of an inefficient mode of HIV-1 entry in trophoblasts, spreading of
the virus to the fetus via infection of trophoblasts is a possible scenario. Indeed, viral production
in trophoblasts could be triggered under natural conditions upon exposure to TNF-α and/or IL-1.
These newly released virions, as we observed when HIV-1-infected trophoblasts were treated
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

22
with TNF-α and co-cultured with PBMCs, could next productively infect underlying susceptible
fetal cells including Hofbauer cells (49).
In line with our results, the relative importance of TNF-α and IL-1 during vertical
transmission of HIV-1 has been indirectly put forward in previous works. First, trophoblastic
cells from HIV-1-infected placentas were found to express higher levels of TNF-α, IL-1β and IL-
6 and such levels also correlated with the amounts of HIV-1 Gag transcripts found in
trophoblastic cells (49, 50). Second, pre-treatment of trophoblastic cells with TNF-α and IL-1β
increased lymphocytic cell adhesion to trophoblastic cells (51). Third, cell contact between
macrophages and trophoblasts resulted in up-regulation of HIV-1 expression that was mediated
by the release of TNF-α and IL-6 by macrophages (52). Based on these published data together
with the present findings, it can be proposed that TNF-α and IL-1 are produced by HIV-1-
infected trophoblastic cells and/or macrophages upon cell contact with trophoblasts. As a
consequence, these cytokines would in turn up-regulate HIV-1 LTR activity and virus production.
This may represent a potential mechanism of HIV-1 replication in trophoblastic cells leading
ultimately to vertical transmission.
TNF-α was able to activate HIV-1 LTR-driven transcriptional activity in trophoblast cells at a
concentration as low as 1 ng/ml. The physiological significance of such findings is provided by
the demonstration that TNF-α was reported to range from 1.1 to 2.8 ng/ml in placental
supernatants and from 3.9 to 8.5 ng/ml in decidual supernatants (53). IL-1α and IL-1β, on the
other hand, triggered significant activation of the regulatory elements of HIV-1 at a concentration
up to a 100-fold less than TNF-α. Considering that IL-1 was previously reported to be at a
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

23
concentration of 0.19 ng/ml at term and 0.68 ng/ml at the onset of labor (54), it can be proposed
that IL-1 is also an extremely potent activator of HIV-1’s LTR in trophoblastic cells. Moreover,
the strong effect mediated by TNF-α and IL-1 on LTR activity was neither cell line- nor clade-
specific, therefore providing credence to the observed phenomenon. At the molecular level, the
cytokine-mediated augmentation of HIV-1 transcriptional activity appears to be mediated via the
ubiquitous mammalian transcriptional factor NF-κB. The TNF-α-dependent signalling pathway
has been extensively studied in lymphocytic and monocytic cells and NF-κB is thought to play a
key role in triggering HIV-1 expression in these cells, which are considered as major cellular
reservoirs of this retrovirus (28).
The roles played by TNF-α during gestation are thought to include: control of cell migration
and placental growth, cell death, immune privilege, hormone production (progesterone,
oestradiol, hCG) and parturition (55-57). It is interesting to note that both TNF-α and IL-1 exert
their effect primarily at the onset of pregnancy and again during labour (25, 53, 58-65).
Interestingly, it coincides with the timing of a higher risk of HIV-1 vertical transmission (7, 11).
Moreover, concomitant viral and bacterial infections are among the risk factors associated with
vertical transmission of HIV-1 (66). Given that certain microbial infections lead to a transient
expression of IL-1 and TNF-α during pregnancy (67), it is tempting to speculate that the presence
of pro-inflammatory cytokines creates conditions leading to higher HIV-1 expression and thus an
increased probability of its vertical transmission.
Taken together, the data presented in this report provide important novel pieces of information
in regard to the possible mechanism of in utero transmission of HIV-1. We have shown that HIV-
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

24
1 enters massively into trophoblastic cells and data from infection studies with VSV-G
pseudotypes HIV-1 particles suggest that there are no other intracellular restrictions in this cell
type. The natural low susceptibility of trophoblast cells to a productive HIV-1 infection is linked
with a block at the initial stage(s) of the virus life cycle and more precisely with a vesicular
uptake of p24, a process that leads to degradation by lysosomal enzymes and/or transcytosis of
the virus. We further show that these limitations can be partially overcome by a treatment with
pro-inflammatory cytokines such as TNF-α and IL-1. The expression profile of these cytokines
suggest that productive HIV-1 infection of trophoblasts may be favoured at two different time
points during the course of pregnancy, i.e. first at the onset of pregnancy, where there are highly
proliferative and invasive trophoblastic cells, and later at term. Since there is a limited time frame
of TNF-α and IL-1 expression and a bias towards Th2-type cytokine expression during
pregnancy, this may help to explain in part why HIV-1 transmission may be limited during
pregnancy. by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

25
ACKNOWLEDGEMENTS
We thank Dr. M. Dufour for technical assistance in flow cytometry studies. This study was
supported by a grant to M.J.T. from the Canadian Institutes of Health Research (CIHR)
HIV/AIDS Research Program (Grants #HOP-15575). This work was performed by G.V. in
partial fulfillment of her Ph.D. Degree in the Program of Microbiology-Immunology, Faculty of
Medicine, Laval University. G.V. and M.R.T. are recipients of CIHR Doctoral Research Awards
from the HIV/AIDS Research Program and M.J.T. holds a Tier 1 Canada Research Chair in
Human Immuno-Retrovirology.
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

26
REFERENCES
1. Dabis, F., Msellati, P., Dunn, D., Lepage, P., Newell, M. L., Peckham, C., and Van de
Perre, P. (1993) Aids 7, 1139-1148
2. Blanche, S., Rouzioux, C., Moscato, M. L., Veber, F., Mayaux, M. J., Jacomet, C.,
Tricoire, J., Deville, A., Vial, M., Firtion, G., and et al. (1989) N Engl J Med 320, 1643-
1648
3. Zachar, V., Zacharova, V., Fink, T., Thomas, R. A., King, B. R., Ebbesen, P., Jones, T. B.,
and Goustin, A. S. (1999) AIDS Res Hum Retroviruses 15, 1673-1683
4. Thiry, L., Sprecher-Goldberger, S., Jonckheer, T., Levy, J., Van de Perre, P., Henrivaux,
P., Cogniaux-LeClerc, J., and Clumeck, N. (1985) Lancet 2, 891-892
5. Lepage, P., Van de Perre, P., Carael, M., Nsengumuremyi, F., Nkurunziza, J., Butzler, J.
P., and Sprecher, S. (1987) Lancet 2, 400
6. Willumsen, J. F., Newell, M. L., Filteau, S. M., Coutsoudis, A., Dwarika, S., York, D.,
Tomkins, A. M., and Coovadia, H. M. (2001) Aids 15, 1896-1898
7. Rouzioux, C., Costagliola, D., Burgard, M., Blanche, S., Mayaux, M. J., Griscelli, C., and
Valleron, A. J. (1995) Am J Epidemiol 142, 1330-1337
8. Lewis, S. H., Reynolds-Kohler, C., Fox, H. E., and Nelson, J. A. (1990) Lancet 335, 565-
568
9. Mano, H., and Chermann, J. C. (1991) AIDS Res Hum Retroviruses 7, 83-88
10. Soeiro, R., Rubinstein, A., Rashbaum, W. K., and Lyman, W. D. (1992) J Infect Dis 166,
699-703
11. Courgnaud, V., Laure, F., Brossard, A., Bignozzi, C., Goudeau, A., Barin, F., and
Brechot, C. (1991) AIDS Res Hum Retroviruses 7, 337-341
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

27
12. Lagaye, S., Derrien, M., Menu, E., Coito, C., Tresoldi, E., Mauclere, P., Scarlatti, G.,
Chaouat, G., Barre-Sinoussi, F., and Bomsel, M. (2001) J Virol 75, 4780-4791
13. De Andreis, C., Simoni, G., Rossella, F., Castagna, C., Pesenti, E., Porta, G., Colucci, G.,
Giuntelli, S., Pardi, G., and Semprini, A. E. (1996) Aids 10, 711-715
14. Martin, A. W., Brady, K., Smith, S. I., DeCoste, D., Page, D. V., Malpica, A., Wolf, B.,
and Neiman, R. S. (1992) Hum Pathol 23, 411-414
15. Backe, E., Jimenez, E., Unger, M., Schafer, A., Jauniaux, E., and Vogel, M. (1992) J Clin
Pathol 45, 871-874
16. Chandwani, S., Greco, M. A., Mittal, K., Antoine, C., Krasinski, K., and Borkowsky, W.
(1991) J Infect Dis 163, 1134-1138
17. Zachar, V., Thomas, R. A., Jones, T., and Goustin, A. S. (1994) Aids 8, 129-130
18. Menu, E., Mbopi-Keou, F. X., Lagaye, S., Pissard, S., Mauclere, P., Scarlatti, G., Martin,
J., Goossens, M., Chaouat, G., Barre-Sinoussi, F., and M'Bopi Keou, F. X. (1999) J Infect
Dis 179, 44-51
19. Tscherning-Casper, C., Papadogiannakis, N., Anvret, M., Stolpe, L., Lindgren, S., Bohlin,
A. B., Albert, J., and Fenyo, E. M. (1999) J Virol 73, 9673-9678
20. Vidricaire, G., Tremblay MJ. (In press, 2003) Médicine Science
21. Al-Harthi, L., Guilbert, L. J., Hoxie, J. A., and Landay, A. (2002) AIDS Res Hum
Retroviruses 18, 13-17
22. David, F. J., Autran, B., Tran, H. C., Menu, E., Raphael, M., Debre, P., Hsi, B. L.,
Wegman, T. G., Barre-Sinoussi, F., and Chaouat, G. (1992) Clin Exp Immunol 88, 10-16
23. David, F. J., Tran, H. C., Serpente, N., Autran, B., Vaquero, C., Djian, V., Menu, E.,
Barre-Sinoussi, F., and Chaouat, G. (1995) Virology 208, 784-788
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

28
24. Mognetti, B., Moussa, M., Croitoru, J., Menu, E., Dormont, D., Roques, P., and Chaouat,
G. (2000) Clin Exp Immunol 119, 486-492
25. Robertson, S. A., Seamark, R. F., Guilbert, L. J., and Wegmann, T. G. (1994) Crit Rev
Immunol 14, 239-292
26. Saito, S. (2000) J Reprod Immunol 47, 87-103.
27. Norwitz, E. R., Schust, D. J., and Fisher, S. J. (2001) N Engl J Med 345, 1400-1408
28. Poli, G., Fauci, A.S. (1995) in In: Human cytokines: their role in disease and therapy, pp.
421-449, Blackell Scientific Publications, Inc.
29. Vidricaire, G., Tremblay M.J. (In press, 2003) in 10th Conference on Retroviruses and
Opportunistic Infections (CROI), Boston, MA
30. Canki, M., Thai, J. N., Chao, W., Ghorpade, A., Potash, M. J., and Volsky, D. J. (2001) J
Virol 75, 7925-7933
31. Lahm, H. W., and Stein, S. (1985) J Chromatogr 326, 357-361.
32. Azocar, J., and Essex, M. (1979) Cancer Res 39, 3388-3391.
33. Connor, R. I., Chen, B. K., Choe, S., and Landau, N. R. (1995) Virology 206, 935-944.
34. Yee, J. K., Miyanohara, A., LaPorte, P., Bouic, K., Burns, J. C., and Friedmann, T. (1994)
Proc Natl Acad Sci U S A 91, 9564-9568.
35. Henderson, A. J., Zou, X., and Calame, K. L. (1995) J Virol 69, 5337-5344.
36. Jeeninga, R. E., Hoogenkamp, M., Armand-Ugon, M., de Baar, M., Verhoef, K., and
Berkhout, B. (2000) J Virol 74, 3740-3751.
37. Chen, B. K., Saksela, K., Andino, R., and Baltimore, D. (1994) J Virol 68, 654-660.
38. Fortin, J. F., Cantin, R., Lamontagne, G., and Tremblay, M. (1997) J Virol 71, 3588-3596.
39. Bounou, S., Leclerc, J. E., and Tremblay, M. J. (2002) J Virol 76, 1004-1014.
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

29
40. Barbeau, B., Bernier, R., Dumais, N., Briand, G., Olivier, M., Faure, R., Posner, B. I., and
Tremblay, M. (1997) J Biol Chem 272, 12968-12977.
41. Zachar, V., Spire, B., Hirsch, I., Chermann, J. C., and Ebbesen, P. (1991) J Virol 65,
2102-2107
42. Marechal, V., Clavel, F., Heard, J. M., and Schwartz, O. (1998) J Virol 72, 2208-2212
43. Schaeffer, E., Geleziunas, R., and Greene, W. C. (2001) J Virol 75, 2993-3000
44. Zachar, V., Fink, T., Koppelhus, U., and Ebbesen, P. (2002) AIDS Res Hum Retroviruses
18, 839-847
45. Benkirane, M., Chun, R. F., Xiao, H., Ogryzko, V. V., Howard, B. H., Nakatani, Y., and
Jeang, K. T. (1998) J Biol Chem 273, 24898-24905
46. El Kharroubi, A., Piras, G., Zensen, R., and Martin, M. A. (1998) Mol Cell Biol 18, 2535-
2544
47. Miller, S. C., Taylor, A., Watanabe, K., Mok, K., and Torti, F. M. (1997) Exp Cell Res
230, 9-21
48. Okada, M., and Jeang, K. T. (2002) J Virol 76, 12564-12573
49. Plaud-Valentin, M., Delgado, R., Garcia, V., Zorrilla, C., Gandia, J., and Melendez-
Guerrero, L. M. (1999) Cell Mol Biol (Noisy-le-grand) 45, 423-431
50. Lee, B. N., Ordonez, N., Popek, E. J., Lu, J. G., Helfgott, A., Eriksen, N., Hammill, H.,
Kozinetz, C., Doyle, M., Kline, M., Langston, C., Shearer, W. T., and Reuben, J. M.
(1997) J Virol 71, 3628-3635
51. Douglas, G. C., Hu, J., Thirkill, T. L., Hovanes, K., Sharma, S., and King, B. F. (1994) J
Reprod Immunol 27, 49-62
52. Bacsi, A., Csoma, E., Beck, Z., Andirko, I., Konya, J., Gergely, L., and Toth, F. D. (2001)
J Interferon Cytokine Res 21, 1079-1088
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

30
53. Jaattela, M., Kuusela, P., and Saksela, E. (1988) Lab Invest 58, 48-52
54. Opsjln, S. L., Wathen, N. C., Tingulstad, S., Wiedswang, G., Sundan, A., Waage, A., and
Austgulen, R. (1993) Am J Obstet Gynecol 169, 397-404
55. Yang, Y., Yelavarthi, K. K., Chen, H. L., Pace, J. L., Terranova, P. F., and Hunt, J. S.
(1993) J Immunol 150, 5614-5624.
56. Yui, J., Garcia-Lloret, M., Wegmann, T. G., and Guilbert, L. J. (1994) Placenta 15, 819-
835
57. Yui, J., Hemmings, D., Garcia-Lloret, M., and Guilbert, L. J. (1996) Biol Reprod 55, 400-
409
58. Paulesu, L., King, A., Loke, Y. W., Cintorino, M., Bellizzi, E., and Boraschi, D. (1991)
Lymphokine Cytokine Res 10, 443-448
59. Hu, X. L., Yang, Y., and Hunt, J. S. (1992) J Reprod Immunol 22, 257-268
60. Phillips, T. A., Ni, J., and Hunt, J. S. (2001) Placenta 22, 663-672
61. Chen, H. L., Yang, Y. P., Hu, X. L., Yelavarthi, K. K., Fishback, J. L., and Hunt, J. S.
(1991) Am J Pathol 139, 327-335.
62. Pijnenborg, R., McLaughlin, P. J., Vercruysse, L., Hanssens, M., Johnson, P. M., Keith, J.
C., Jr., and Van Assche, F. A. (1998) Placenta 19, 231-239
63. Hunt, J. S., Chen, H. L., Hu, X. L., and Tabibzadeh, S. (1992) Biol Reprod 47, 141-147
64. Tabibzadeh, S. (1991) Am J Reprod Immunol 26, 1-4
65. Knofler, M., Mosl, B., Bauer, S., Griesinger, G., and Husslein, P. (2000) Placenta 21,
525-535.
66. St Louis, M. E., Kamenga, M., Brown, C., Nelson, A. M., Manzila, T., Batter, V., Behets,
F., Kabagabo, U., Ryder, R. W., Oxtoby, M., and et al. (1993) Jama 269, 2853-2859
67. Raghupathy, R. (1997) Immunol Today 18, 478-482
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

31
FIGURE LEGENDS
Figure 1. HIV-1 enters massively in trophoblastic cells. JAR cells were exposed to VSV-G
pseudotypes (panel A), Ada-M pseudotypes (panel B), or complete NL4-3 viruses for 5 min to 4
h at 370C. The cells were then washed, trypsinised and lysed. The process of virus entry was
measured by evaluating the amount of p24 in the cell lysates. Data shown are expressed as the
means +/- standard deviations of triplicate samples and are representative of three independent
experiments.
Figure 2. Intracellular p24 is primarily localized in endosomal vesicles in trophoblastic cells.
JAR (panel A) and PM1 cells (panel B) were exposed to HIV-1 particles pseudotyped with Ada-
M envelope glycoproteins for the indicated time periods at 37°C. After viral exposure, cells were
washed, trypsinised and resuspended in a swelling buffer. Cells were next disrupted by dounce
homogenization and levels of p24 were evaluated in each cellular fraction. Data shown are
expressed as the means +/- standard deviations of triplicate samples and are representative of
three independent experiments.
Figure 3. HIV-1 transcriptional activity is increased upon treatment of trophoblasts with TNF-α
and IL-1β. JAR cells were infected with HIV-1 reporter viruses bearing M-tropic (panels A and
B) or T-tropic (panels C and D) envelope glycoproteins and were either left untreated or treated
with increasing doses of TNF-α (panels A and C) or IL-1β (panels C and D). Cells were lysed at
24 h post-stimulation and HIV-1-encoded luciferase activity was monitored in each cell lysate.
Values from the luminometer are expressed as Relative Light Units (RLU). Data shown are
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

32
expressed as the means +/- standard deviations of quadruplicate samples and are representative of
three independent experiments. Fold increase over untreated cells is indicated at the top of each
data point.
Figure 4. Cytokine-mediated increase in HIV-1 LTR activity is dose-dependent in trophoblasts.
JAR cells were first infected with HIV-1 particles bearing VSV-G envelope glycoproteins and
were either left untreated or treated with increasing doses of TNF-α (panel A), IL-1α (panel B),
or IL-1β (panel C). Cells were lysed either at 8 h (panel C) or 24 h (panels A and B) post-
stimulation and HIV-1-encoding luciferase activity was assessed in each cell lysate. Values from
the luminometer are expressed as Relative Light Units x 103 (kRLU). Data shown are expressed
as the means +/- standard deviations of quadruplicate samples and are representative of three
independent experiments.
Figure 5. Cytokine-mediated induction of HIV-1 transcription is also seen in BeWo trophoblastic
cells. BeWo cells were inoculated with VSV-G pseudotypes and were either left untreated or
treated with TNF-α (panel A), IL-1α (panel B), or IL-β (panel C). Cells were lysed at 24 h post-
stimulation and HIV-1-encoded luciferase activity was monitored in each cell lysate. Values from
the luminometer are expressed as Relative Light Units x 103 (kRLU). Data shown are expressed
as the means +/- standard deviations of quadruplicate samples and are representative of three
independent experiments. Fold increase over untreated cells is indicated at the top of each bar.
Figure 6. Production of fully infectious HIV-1 particles is seen when virus-infected trophoblasts
are treated with TNF-α and co-cultured with indicator cells. JAR cells were inoculated with fully
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

33
infectious NL4-3 virions and were either left untreated or treated with TNF-α at 10 ng/ml. The
infected JAR cells were next co-cultured for 24 h with indicator LuSIV cells (panel A) or primary
human PBMCs (panel B). Luciferase activity in the indicator LuSIV cell line was measured on
day 3, 5, 7, 9 and 12 post-coculture (panel A), while levels of p24 were evaluated in cell-free
culture media from PBMCs on day 1, 3, 5, 7, 9 and 12 post-coculture (panel B). Luciferase
activity is depicted as Relative Light Units x 103 (kRLU). Data shown are expressed as the means
+/- standard deviations of quadruplicate samples and are representative of three independent
experiments.
Figure 7. Limited HIV-1 infection in trophoblast cells is not related to intracellular restrictions
other than the route of virus entry. JAR cells were inoculated with complete NL4-3 virions
pseudotyped with VSV-G envelope glycoproteins and were left untreated or treated with TNF-α
at 10 ng/ml. Cell-free culture media were collected on day 1, 2, 3, 5, and 7 days post-stimulation
and levels of p24 were evaluated. Levels of p24 were monitored in cell-free culture media at the
indicated time periods. Data shown are expressed as the means +/- standard deviations of
quadruplicate samples and are representative of three independent experiments.
Figure 8. Different HIV-1 LTR subtypes are transactivated by TNF-α and IL-1β in trophoblasts.
JAR cells were co-transfected with an expression vector coding for the luciferase reporter gene
under the control of an HIV-1 LTR subtype and an actin-driven β-galactosidase vector. Cells
were next either left untreated or treated with TNF-α or IL-1β and were lysed at 8 h post-
stimulation. HIV-1-encoded luciferase activity and actin-dependent β-galactosidase value were
monitored in each cell lysate. Standardization of the luciferase counts was achieved by dividing
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

34
each luciferase activity mean value by the measured β-galactosidase activity mean value. Data
shown are from quadruplicate samples and are representative of three independent experiments.
Fold increase over untreated cells is indicated at the top of each bar.
Figure 9. Cytokine-dependent transactivation of HIV-1 LTR in trophoblasts is mediated via NF-
κB. JAR cells were transiently transfected with pLTR-Luc, pmκBLTR-Luc, or pNF-κB-Luc and
were either left untreated or treated with TNF-α. Cells were lysed at 8 h post-stimulation and
luciferase activity was monitored in each cell lysate. Values from the luminometer are expressed
as Relative Light Units (RLU). Data shown are expressed as the means +/- standard deviations of
quadruplicate samples and are representative of three independent experiments. Fold increase
over untreated cells is indicated at the top of each bar.
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

0
10
20
30
40
50
60
70
80
90
100
5 min 15 min 30 min 1 h 2 h 4 h
Vira
l Ent
ry (
ng/m
l of p
24)
Ada-M
A
B
C
0
5
10
15
20
25
30
35
40
5 min 15 min 30 min 1 h 2 h 4 h
NL4-3
Vira
l Ent
ry (
ng/m
l of p
24)
0
10
20
30
40
50
60
70
80
90
100
5 min 15 min 30 min 1 h 2 h 4 h
VSV-G
Vira
l Ent
ry (
ng/m
l of p
24)
Figure 1
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

0
400
800
1200
1600
2000
5 min 30 min 60 min 120 min
JAR
0
400
800
1200
1600
2000
5 min 30 min 60 min 120 min
PM1
A
B
100%97%
82%
70%
63%
65%
p24
(pg/
ml)
p24
(pg/
ml)
Cytosol Vesicles
35%37%30%
18%
Ada-M
Ada-M
Figure 2
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

C
0.0
2.0
4.0
6.0
8.0
10.0
0 0.01 0.1 1 10 100
Luciferase Activity (RLU)Lu
cife
rase
Act
ivity
(RLU
) HXB-2 with TNF-α
0.6X 0.6X
4.3X4.2X
4.7X
TNF-α (ng/ml)
0.0
20.0
40.0
60.0
80.0
100.0
120.0
0 0.01 0.1 1 10 100
.0Luciferase Activity (RLU)
Luci
fera
se A
ctiv
ity (R
LU)
A
Ada-M with TNF-α
1.4X 1.1X
18.6X
87.3X
48.5X
TNF-α (ng/ml)
0.0
4.0
8.0
12.0
16.0
20.0
0 0.002 0.02 0.2 2 20
Luciferase Activity (RLU)
Luci
fera
se A
ctiv
ity (R
LU)
B
Ada-M with IL-1β
1.2X5.4X
26.3X22.6X
16.2X
IL-1β (ng/ml)
Luciferase Activity (RLU)
Luci
fera
se A
ctiv
ity (R
LU) HXB-2 with IL-1b
1.5X 1.6X
14.5X
19X
1.5X
0.0
2.0
4.0
6.0
8.0
10.0
12.0
0 0.002 0.02 0.2 2 20
D
IL-1β (ng/ml)
HXB-2 with IL-1β
Figure 3
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

0.0
10.0
20.0
30.0
40.0
50.0
60.0
70.0
0 0.01 0.1 1 10 100
Dose (ng/ml)
TNF-α
Luci
fera
se A
ctiv
ity (k
RLU
)
A
0.0
10.0
20.0
30.0
40.0
50.0
60.0
0 0.02 0.2 2 20 200
Dose (ng/ml)
IL-1β
Luci
fera
se A
ctiv
ity (k
RLU
)
C
0.0
10.0
20.0
30.0
40.0
50.0
0 0.01 0.1 1 10 100
Dose (ng/ml)
IL-1α
Luci
fera
se A
ctiv
ity (k
RLU
)
B
Figure 4
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

0.0
0.4
0.8
1.2
1.6
2.0
TNF-α (ng/ml)
0
0.1
1
10Lu
cife
rase
Act
ivity
(kR
LU)
ABeWo
3.5X
5.4X
8.2X
0.0
0.2
0.4
0.6
0.8
1.0
IL-1β (ng/ml)
0
0.02
0.2
2
Luci
fera
se A
ctiv
ity (
kRLU
)
C
BeWo
1.8X
4.2X 4.0X
0.0
0.2
0.4
0.6
0.8
1.0
1.2
IL-1α (ng/ml)
0
0.01
0.1
1
Luci
fera
se A
ctiv
ity (k
RLU
)
BBeWo
2.3X
3.9X
4.4X
Figure 5
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

Vira
l Pro
duct
ion
(ng
of p
24)
Luci
fera
se A
ctiv
ity (k
RLU
)
A
B
0.0
3.0
6.0
9.0
12.0
15.0
3 5 7 9 12
Time Course (day)
Mock-infected
Mock-infected/TNF-α
Infected NL4-3Infected NL4-3/TNF-α
0.0
0.6
1.2
1.8
2.4
3.0
3.6
4.2
1 3 5 7 9 12Time Course (day)
Mock-infected
Mock-infected/TNF-α
Infected NL4-3
Infected NL4-3/TNF-α
Figure 6
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

Figure 7
0.0
500.0
1000.0
1500.0
2000.0
2500.0
1 2 3 5 7
Time Course (day)
Mock-infected
Mock-infected/TNF-α
Infected VSV (NL4-3)
Infected VSV (NL4-3)/TNF-α
Vira
l Pro
duct
ion
(ng
of p
24)
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

1.4X
4.8X
1.5X
2.9X3.2X
5.4X
2.1X
3.8X
1.4X
1.8X
2.6X
4.6X
2.8X
7.8X
0.00
0.20
0.40
0.60
0.80
1.00
1.20
Clade A Clade B Clade C Clade D Clade E Clade F Clade G
Untreated
TNF-α
IL-1β
Luci
fera
se a
ctiv
ity n
orm
aliz
ed in
β-g
alac
tosi
dase
val
ue
Figure 8
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

Luci
fera
se A
ctiv
ity (R
LU)
1X
4.4X
7.4X
1.2X
0
30
60
90
120
150
Mock-transfected
LTR-Luc mκB-LTR-Luc NFκB-Luc
Without TNF-α
With TNF-α
Figure 9
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

Spontaneous Luciferase Activity (RLU)
Mock-Infected
Table 1 : Susceptibility of Trophoblastic Cell Lines to HIV-1 Infection with Ada-M, HXB-2 and VSV-G Pseudotypes
Luciferase acitivty is expressed in RLU. Results shown are expressed as means ± standard deviations of quadruplate samples and are representative of three experiments.
JAR
JEG-3
0.4 ± 0.07
0.5 ± 0.07
BeWo 0.4 ± 0.03
1.1 ± 0.11
0.5 ± 0.06
0.4 ± 0.02
1.1 ± 0.53
0.3 ± 0.07
0.4 ± 0.03 207.2 ± 28.53
605.9 ± 15.00
281.5 ± 13.73
Ada-Mpseudotype
HXB-2pseudotype
VSV-Gpseudotype
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from

Gaël Vidricaire, Mélanie R Tardif and Michel J Tremblay and IL-1αpro-inflammatory cytokines TNF-
theinternalization of the human immunodefiency virus type 1 and can be overcome by The low viral production in trophoblastic cells is due to a high endocytic
published online February 25, 2003J. Biol. Chem.
10.1074/jbc.M210470200Access the most updated version of this article at doi:
Alerts:
When a correction for this article is posted•
When this article is cited•
to choose from all of JBC's e-mail alertsClick here
by guest on April 6, 2018
http://ww
w.jbc.org/
Dow
nloaded from