IPF model - SMC Laboratories
Transcript of IPF model - SMC Laboratories

Ver. 2021.1 1
IPF model-SMC’s CRO services-
smccro-lab.com
SMC Laboratories, Inc.

29Source: IPF guideline from ATS/ERS/JRS/ALAT, 2010
Treatment / Drug Mechanism of action Route Animal modelGuideline recommendation
/evidence quality
Recommended in selected patients
Lung transplantationReplacement of fibrotic lung with
donor lungSurgery - Strongly/Low
Supplemental oxygen Reduction of hypoxemia Inhalation - Strongly/Very low
Acetylcysteine
monotherapyAnti-oxidant Oral, Inhalation
BLM (i.t.)
/prophylactic regimenWeakly/Low
Corticosteroid + AZA +
acetylcysteineImmunosuppressant + antioxidant Oral - Weakly/Low
PirfenidoneAnti-inflammatory + antifibrptic +
antioxidantOral
BLM( i.v.)
/prophylactic and
therapeutic regimen
Weakly/Low-to-moderate
Anticoagulation Anticoagulant OralBLM (i.t.)
/prophylactic regimenWeakly/Very low
Not recommended
Bosentan Endothelin receptor antagonist OralBLM (i.t.)
/prophylactic regimenStrongly not/Moderate
Corticosteroid
monotherapyImmunosuppressant Oral
BLM (i.t.)
/prophylactic regimenStrongly not/Very low
Corticosteroid +
immunomodulatorImmunosuppressant Oral - Strongly not/Low
EnterceptRecombinant soluble human TNF
receptorSC
BLM (i.t.), Silica (i.t.)
/prophylactic regimenStrongly not/Moderate
Interferon-gamma Immunomodulator IV BLM (unknown) Strongly not/High
Current therapies for IPF

39Source: clinicaltrial.gov
Company Drug Target/mechanism Route Period Endpoint Stage
Intermune PirfenidoneTGF-β signaling
Oral 72 weeks1)FVC
P3 finishedAnti-inflammatory 2)PFS, 6MWT etc.
Boehringer Ingelheim BIBF 1120FGFR, PDGFR,
VEGFROral 52 weeks
1)FVCP3 finished
2)SGRQ, SOBQ, etc.
Actelion ACT-064992 dual ERA Oral12
months
1)FVCP2 finished
Fibrogen FG-3019 CTGF IV 48 weeks1)FVC
P22)Fibrosis area
Centocor CNTO 888 CCL2 IV 48 weeks1)Pulmonary function and safety
P22)Clinical outcomes
MedImmune Tralokinumab IL-13 SC 72 weeks1)FVC
P22)Safety and clinical outcomes
Sanofi-Aventis SAR156597 IL-13/IL-4 SC 22 weeks1)Safety and tolerability
P22)FVC, DICO and dyspnea score
Gilead SciencesGS-6624
LOXL2 IV182
weeks
1)PFSP2
(Simtuzumab) 2)All-cause mortality
Bristol-Myers Squibb BMS-986020 LPA1 Oral 26 weeks1)FVC
P22)Safety
Hoffmann-La Roche Lebrikizumab IL-13 SC 2.5 years1)PFS
P22)FVC, 6MWT, etc.
GlaxoSmithKline GSK2126458 PI3K/mTOR Oral7 to 10
days
1)PD/PKP2
2)Safety and tolerability
Biogen(Stromedix) STX-100 αvβ6 integrin SC 24 weeks1)Safety
P22)FVC, HRCT assessment, etc.
Hoffmann-La Roche vismodegib SMO antagonist Oral Week 521)FVC
P22)DLCO
Promedior PRM-151 PTX-2 IV --
P1
GenzymeGC1008
TGF-β 1, 2 and 3 IV 3 years1)Safety and tolerability
P1(Fresolimumab) 2)Clinical outcomes
ImmuneWorks IW001 Col (V) Oral 24 week1)Safety and tolerability
P12)biologic effects
Drug candidates in clinical trials

4
Inflammation phase Fibrosis phase
BLM i.t.Day 0 Day 7 Day 14 Day 21 Day 28
Direct damageinitially to alveolar epithelial cells
Fibroblast proliferation Extracellular matrix synthesize Maximal responses
Development of fibrosis(biochemically and histologically)
Increase of ・neutrophils・lymphocytes
Marios A, et al., Current Opinion in Pulmonary Medicine. 17:355-361, 2011
■ Variation of the bleomycin animal model
Route of
administrationDose Advantage Disadvantage
Intratracheal (i.t.) 1.25 - 4 U/kg
Direct damage to alveolar epithelial.
The most common route of administration.
Only single instillation needed.
Short time frame for disease development.
High reproducibility.
Self-limiting response after 28 days.
High mortality.
Intravenous (i.v.) 30 U/kg, twice per week1ry damage to endothelium.
Subpleural fibrosis.
Not applicable in all animals.
Long time frame to disease development.
Intraperitoneal (i.p.) 15 - 35 U/kg1ry damage to endothelium.
Subpleural fibrosis.Multiple doses required.
Subcutaneous (s.c.) 150 U/kgResembles the progressive nature of fibrosis.
for a short time frame.
Daily injections/micro-osmotic pump
installation required
Also induced skin fibrosis.
Animal model for IPF: BLM-induced pulmonary fibrosis

5
-Sampling scheme allowing all analyses in a single mouse (histology, gene expression,
biochemistry and BALF analysis)
-Bleomycin-induced model optimized for evaluation of fibrosis severity, body weight loss
and mortality
-Increased reproducibility and uniform phenotype enabled by the use of Microsprayer
-Expert histology based on the knowledge of fibrotic/inflammatory diseases
-In-life evaluation of fibrotic lesions by CT scan as in clinical studies
- Availability of positive control – Dexamethasone and Nintedanib
■ SMC’s IPF model offers
■ Performance
■ Over 80 test substances have been evaluated
■ Both small-molecule compounds and antibodies were experienced
Advantages of SMC’s IPF model

69
Mean ± SEM
■ Uniform distribution by MicroSprayer®■ Dose optimization (Body weight)
■ Survival rate (3.0 mg/kg BLM)
Optimization of BLM model

79
■ After BALF collection, left and post-caval lobe bronchus are ligated to avoid leakage of the instilled fixative. Then, three
fixed lobes (for histological analyses) and two unfixed lobes (for gene expression analysis and collagen assay) are
harvested from each mouse.
SMC’s advantage: Sampling scheme and technique

8
Score: 1
x100 x400
x100 x400
Score: 3
x100
x400
Score: 5
Ashcroft score is
■ simple method of estimating severity of pulmonary fibrosis using MT-stained section
■ widely used in pharmacological study for anti-fibrotic efficacy in BLM model
x100
■ Representative microphotographs of MT stained lung sections
Key endpoint: Ashcroft score

9
Day 14 Day 21
PB
S i.t
BLM
i.t
:Fibrotic lesion
right left
anterior
posterior
Region of Interest (ROI)
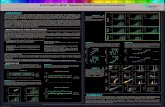
■ High resolution CT (HRCT) scan shows increasing interstitial fibrotic lesions in the same mice
■ Hounsfield unit (fibrotic density) of the ROI is increased in BLM model time-dependent manner
Day 21 BLM i.t
Lung field Lung field
Lung field Lung field
■ Micro-CT imaging
Key endpoint: CT scan

10
■ BALF total cells were increased at inflammatory phase (Day7) and early fibrosis phase (Day 14), then decreased at late fibrosis
phase (Day21)
■ Lung hydroxyproline content significantly increased at late fibrosis phase (Day 21)
■ Ashcroft score were increased as well as hydroxyproline content
■ Collagen Type 1 gene were increased as well as Ashcroft score and hydroxyproline content and TIMP-1 gene were increased at
fibrosis phase (Day 14 and Day 21)
■ Disease progression of BALF total cells, hydroxyproline content, Ashcroft score and fibrosis-related
genes
Parameters: Time course of disease progression
Co
ntr
ol
Day 7
Day 1
4
Day 2
1
0
100
200
300
400
To
tal c
ell
(x1
04 c
ells
)
**
**
BLM
Co
ntr
ol
Day 7
Day 1
4
Day 2
1
0
1
2
3
4
5
Rela
tive q
uan
tity
**
BLM
****
Co
ntr
ol
Day 7
Day 1
4
Day 2
1
0
10
20
30
40
50
Rela
tive q
uan
tity
**
BLM
**
TIMP-1 geneCollagen Type 1 gene
Co
ntr
ol
Day 7
Day 1
4
Day 2
10
20
40
60
80
100L
un
g h
yd
rox
yp
rolin
e(µ
g/le
ft lu
ng
)**
BLM
Co
ntr
ol
Day 7
Day 1
4
Day 2
1
0
1
2
3
4
As
hc
roft
sc
ore
**
**
**
BLM
BALF total cells Lung hydroxyproline
content
Ashcroft score Gene expression

11
■ TGF- and TIMP-1 proteins, fibrosis makers, are increased in BLM model (Day 21)
BDL: below detection limit
Parameters: BALF cytokine levels
■ BALF TGF-β and TIMP-1 at Day 21

12
Day 21Day 0 Day 7
(n= 10) Group
1BLM + Vehicle
acclimation
(n= 10) Group
2BLM + dexamethasone 0.25 mg/kg
acclimation
Oral, QD
Oral, QD
Sacrifice
BLM
BLM
BLM: Bleomycin, Oral: Oral administration, QD: Once daily
2. Histopathological analyses
• MT staining (Ashcroft score)
1. Biochemistry
• Lung hydroxyproline content
Day 14
■ Study design
■ Analyses
Prophylactic positive control: Dexamethasone

13
x16x100
Ve
hic
leD
ex
am
eth
as
on
e
■ Ashcroft score in the dexamethasone group significantly decreased compared to the BLM-Vehicle group.
■ The lung hydroxyproline content significantly decreased in the dexamethasone group compared to the BLM-
Vehicle group.
Mean ± SEM
x16x100
Dexamethasone: Ashcroft score and lung hydroxyproline

14
Day 21Day 0 Day 7
(n= 10) Group
1BLM + Vehicle
acclimation
(n= 10) Group
2BLM + Nintedanib 100 mg/kg
acclimation
Oral, QD
Oral, QD
Sacrifice
BLM
BLM
BLM: Bleomycin, Oral: Oral administration, QD: Once daily
Day 14
■ Study design
■ Analyses
Therapeutic positive control: Nintedanib
2. Histopathological analyses
• MT staining (Ashcroft score)
1. Biochemistry
• Lung hydroxyproline content

n.s
Vehicle Nintedanib0
20
40
60
80
Hy
dro
xy
pro
line
(µg
/Le
ft lu
ng
)
P<0.001
Vehicle Nintedanib0
1
2
3
4
As
hc
roft
sc
ore
15
x16x100
Ve
hic
leN
inte
da
nib
■ Ashcroft score in the Nintedanib group was significantly decreased compared to the BLM-Vehicle group.
■ The lung hydroxyproline content did not change in Nintedanib group compared to the BLM-Vehicle group.
Mean ± SEM
x16x100
Nintedanib: Ashcroft score and lung hydroxyproline

16
Computed tomography
(day 21)
Homogeneity of it Sampling technique
Day 21Day 14Day 7 Saline i.t.
Day 0
BLM i.t.Control
(n= 12) Group
1
acclimation
BLM + Positive control(n= 12)
Group
4
Treatment (oral)
Alveolar epithelial damage
BLM + Test substance(n= 12)
Group
3
Treatment (oral/ i.v./ i.p./ s.c)
BLM + Vehicle(n= 12) Group
2
Treatment (oral/ i.v./ i.p./ s.c)
Alveolar inflammation
Fibrosis
Animal model: Bleomycin (BLM)-induced pulmonary fibrosis model■Animal: C57BL/6J mice, female, week 7-8
■Induction of pulmonary fibrosis: BLM i.t. (microspray) at day 0
Study design
■Aim of the study: To investigate the therapeutic efficacy of test substance on pulmonary fibrosis
■Route of administration: oral/ i.p./ i.v./ s.c.
■Arm: 4
control, vehicle, test substance, positive control (Dexamethasone or Nintedanib)
■The number of mice/group before dosing: n=12
■Baseline: day 0 (just prior to BLM inhalation) and day 6
■Randomization: Body weight at day 0 or day 6
■Treatment period: 2 or 3 weeks
■Endpoints (day 21):
The grade of fibrosis: Ashcroft score (MT staining), Lung hydroxyproline content
<Analytical items>
BAL: cell number, ELISA
Gene expression in the lung
CT (option)
General condition
MT staining (day 21)
Moore BB et al., Am J Physiol Lung Cell Mol Physiol. 2008 (294); L152-60
Kai Y et al., Med Mol Morphol. 2007 (40); 128-40
Study design example: BLM I.T. study

Publications and Presentations
■ Presentations
4. ERS International Congress 2018, “CHIT1 is a novel therapeutic target in idiopathic pulmonary fibrosis
(IPF): anti-fibrotic efficacy of OATD-01, a potent and selective chitinase inhibitor in the mouse model of
pulmonary fibrosis” OncoArendi Therapeutics SA
3. American Thoracic Society 2017 International Conference, “Resokine Modulates Immune Cell
Infiltration into the Lung and Provides Therapeutic Activity in a Bleomycin-Induced Lung Fibrosis Model”
aTyr Pharma, Inc.
2. The 18th International Colloquium on Lung and Airway Fibrosis, “MN-001 (tipelukast), a
nonselective phosphodiesterase, 5-lipoxygenase, leukotriene, phospholipase C and thromboxane A2
inhibitor, demonstrates anti-fibrotic effects in the Bleomycin-induced idiopathic pulmonary fibrosis mouse
model” MediciNova, Inc.
1. American Thoracic Society 2014 International Conference, “Solithromycin Reduces Inflammation In
Mice Caused By Bleomycin-Induced Lung Injury” Cempra Inc.
17