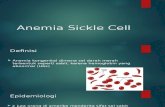
Islet cell structure α cell : glucagon β cell : insulin δcell : somatostatin α cell β cell δcell.
Genetic Modifiers of Sickle Cell Disease - Rio de · PDF fileGenetic Modifiers of Sickle Cell...
-
Upload
duonghuong -
Category
Documents
-
view
266 -
download
2
Transcript of Genetic Modifiers of Sickle Cell Disease - Rio de · PDF fileGenetic Modifiers of Sickle Cell...

Genetic Modifiers of Sickle Cell
Disease
Abdullah Kutlar, MDAbdullah Kutlar, MDAbdullah Kutlar, MDAbdullah Kutlar, MD
Professor of MedicineProfessor of MedicineProfessor of MedicineProfessor of Medicine
Director, Sickle Cell CenterDirector, Sickle Cell CenterDirector, Sickle Cell CenterDirector, Sickle Cell Center

SICKLE CELL DISEASE
� Homozygous state for Hb S
(β6 Glu→Val; GAG→GTG)
� 8-12% of African-Americans carry the Hb S gene
� 1/400 African-American births homozygous for Hb S
� Increased gene frequency in the “malaria belt”
(Africa, Mediterranean, Middle East, India)
� Associated with significant morbidity and mortality

SICKLE CELL DISEASE
� Chronic Hemolytic Anemia
� Vaso-occlusion
� Chronic inflammatory state
� Organ damage

Sickle Cell Disease
Infection/SepsisSplenic SequestrationIschemic StrokeDactylitis
VOEACS
GallstonesPriapism
Fe OverloadAplastic Crisis
Pulmonary HypertensionNephropathyAVNLeg UlcersChronic Lung DiseaseMulti Organ FailureHemorrhagic Stroke
Pediatrics Adults

SICKLE CELL DISEASE: LIFE EXPECTANCY
Male Female
SS 42 48
SC 60 68
Platt, et al. NEJM, 1994;330(23):1639-44

Sickle Cell Disease: Life Expectancy over 3 decades
01020304050
1970 1980 1990 2000
Smith LA, Oyeku SO, Homer C, Zuckerman B. PEDIATRICS. 117(5):1763-1770, 2006

SICKLE CELL DISEASE: PHENOTYPIC HETEROGENEITY

Heterogenity of SCD
� Stroke/CVA – 11% of SS patients up to 20 years of age
� Retinopathy – 3% of SS patients
� Acute Chest Syndrome – 30-50% of SS patients
� Pulmonary hypertension – 20-40% of adult SS patients
� Gallstones – 30-36% of SS patients
� Splenic sequestration – 5-6% up to 6 years of age
� Nephropathy/microalbuminuria – 30%
� Priapism – 6-42% of males with SS
� Avascular Necrosis – 50% at age 35
� Leg ulcers – 4-6% of SS patients > 10 years of age

MODIFIERS OF DISEASE SEVERITY
� α- thalassemia
� High Hb F determinants� Linked ( β-globin haplotypes)
� Unlinked (X-chromosome, others)
� Other genetic factors� Coagulation related polymorphisms
� Endothelial cell function
� Inflammatory mediators
� RBC membrane function
� NO bioavailability
� Others

PHENOTYPIC MODULATION OF SCD: Methodologic Approaches
� Analyses of polymorphisms in candidate genes (SNPs) by high throughput methods
� Genome-wide association studies (GWAS)
� Study of differential gene expression with cDNA microarrays in:� Blood cells (retics, neutrophils, monocytes)
� Bone marrow
� Endothelial cells
� Liver tissue

PHENOTYPIC MODULATION OF SCD
APPROACH:
� Analysis of candidate genes as risk factors for complications of disease
� Comparative study of phenotype in different populations and correlations with genetic factors
� Microarray technology to study differential gene expression
� Design of new therapies based upon new genetic information

APPROACH TO STUDY GENETIC MODIFIERS IN SS
� Study sickle cell patients from distinct populations around the world:
� African-American
� Mediterranean (Italy, Greece,Turkey)
� Asian (Kuwait, India)
� Africa (Nigeria and Kenya)
� South America (Brazil, Caribbean)

APPROACH TO STUDY GENETIC MODIFIERS IN SS
� Phenotypic characterization of distinct sickle cell populations in terms of the frequency of complications/organ damage:
� Stroke risk/CNS disease
� VOE
� Acute chest syndrome
� Avascular necrosis
� Gallstones and cholecystectomy
� Leg ulcers
� Pulmonary hypertension
� Priapism
� Renal disease

EFFECTS OF α-THALASSEMIA INSCD
CELLULAR:
� Decreased MCHC
� Decreased Hb S polymer
� Decreased RBC cation loss
� Decreased RBC density
� Increased RBC deformability

EFFECTS OF α-THALASSEMIA INSCD
HEMATOLOGICAL:
� Reduced Hemolysis
� Decreased Reticulocyte Count
� Increased Hb/Hct
� Decreased MCV

EFFECTS OF α-THALASSEMIA IN
SCD
CLINICAL:
� Increased:� Osteonecrosis
� Splenic sequestration
� Painful episodes (?)
� Decreased:� Cerebrovascular accidents
� Leg ulcers
� Nephropathy/proteinuria
� Longevity

FACTORS INFLUENCING HB F LEVELS IN SCD
� Age
� Gender (F>M)
� βs-globin gene cluster haplotype
� F-cell Production locus (FCP) (Xp22.2)
� Others (Chromosome 6?)

Baseline Hb F levels in SCD
� ~50% variation:
� FCP on Xp22
� -158 C→T at Gγ (Xmn 1 polmorphism)
� ~20-30% variation(12 SNPs in 6q22.2-23.2)
� Phosphodiesterase 7 (PDE7)
� Microtubule associated protein 7 (MAP7)
� Peroxisomal biogenesis factor 7 (PEX7)
� Mitogen activated protein kinase 5 (MAP3K5)

Association Studies in
SCD

AVASCULAR NECROSIS IN SICKLE CELL
DISEASE

AVASCULAR NECROSIS (AVN) OF FEMORAL HEAD IN SCD
RISK FACTORS:
� Alpha thalassemia
� Age
� High hematocrit
� Frequent vaso-occlusive episodes
Ballas et al, Hemoglobin, 13:649,1989
Milner et al, NEJM, 321:1476, 1991

ASSOCIATION STUDIES IN SCD
Phenotype SNP Reference
Osteonecrosis MTHFR Kutlar et al,2001
KL (klotho) Baldwin et al, 2005
BMP6
TGFBR2, 3
EDN1, ECE1

P <0.05
Group
Means & Std Devs
6/6 B 6/7 B 7/7 B
0.0
2.5
5.0
7.5
10.0
Std Dev Mean
Bilirubin Levels and UGT1A1 Polymorphism
p<0.05

Phenotype SNP Reference
Hyperbilirubinemia/ UGT1A1 7/7 Passon et al 2001
Gallstones Fertrin et al, 2003Haverfield et al, 2005
Adekile et al, 2005
ASSOCIATION STUDIES IN SCD

UGT1-A1 POLYMORPHISM IN SCD
� Haverfield et al (Blood; 2005)
� 541 SS patients from Jamaica
� 7/7 genotype associated with higher bilirubin levels
� 7/7 associated with symptomatic gallstones except for younger patients
� Adekile et al (Eur. J. Haematol, 2005)
� 67 SS patients from Georgia (age 2-44)
� Bilirubin levels significantly correlated with Hb F levels and 7/7 genotype in multivariate analyses
� No effect of UGT1-A1 genotype in younger (<10) patients
� No correlation between bilirubin levels and βS-haplotypes and α-thalassemia

ACS

Phenotype SNP Reference
Acute Chest NOS3 T-786C Sharan et al, 2004
NOS1 AAT rep. Sullivan et al, 2001
ASSOCIATION STUDIES IN SCD

Priapus:
In Greek mythology, the god of fertility,
son of Dionysus and Aphrodite,
represented as grotesquely ugly, with
an exaggerated phallus. He was later a
Roman God of gardens,
where his image was frequently
used as a scarecrow.

ASSOCIATION STUDIES IN SCD
Phenotype SNP Reference
Priapism Klotho (KL) Nolan et al, 2004

Pgm: \\Cre_Figure1_MORT.sas Data Lock Date: 31MAR06 Run: 30JUN06
Cumulative Event Rate (%)
0
10
20
30
40
Years Since Randomization
0 1 2 3 4 5 6 7 8 9 10 11 12 13 14

Phenotype SNP ReferenceSurvival/longevity Klotho (KL) Ashley-Koch et al, 2005
TGFBR2NOS2A
ASSOCIATION STUDIES IN SCD

LEG ULCERS IN
SICKLE CELL
DISEASE

Phenotype SNP Reference
Leg ulcers Klotho Steinberg et al, 2005
TEK
SMAD1
SARA1
ASSOCIATION STUDIES IN SCD

Pulmonary Hypertension

Pulmonary Hypertension in SCD
� Prevalence rate – 20-40% in adults
� TR jet velocity ≥ 2.5 m/sec = PASP >30 mm Hg
� Echo results equivalent to right heart cath
� Lower PAP and higher cardiac output than primary PHTN
� Significantly higher mortality rate - 50% in two years

Pulmonary Hypertension in SCD

ASSOCIATION STUDIES IN SCD
Phenotype SNP Reference
Pulmonary Hypertension BMPR2 Koch et al, 2004
ADCY6

Nephropathy in SCD

ASSOCIATION STUDIES IN SCD
Phenotype SNP Reference
Estimated GFR BMPR1B Nolan et al, 2007


ASSOCIATION STUDIES IN SCD
Phenotype SNP Reference
Infection/Bacteremia IGF1R Adewoye et al, 2006
BMP6
TGFBR3
BMPR1A
SMAD6
SMAD 3

Stroke Risk

CONCURRENT STUDIES FOR STROKE RISK
� Taylor, et al. (Blood 2002)� Protective role for VCAM G1238C
(p=0.04, OR = 0.35)
� Hoppe, et al. (Blood, 2004)� IL4R503, TNF-308, ADRB227 (large vessel
stroke)� VCAM1594, LDLR (small vessel stroke)
� Steinberg, et al. (2003)� Klotho (KL) (p=0.006, OR = 2.8)� ECE1 (p<0.0001, OR = 5.2)� TGFBR3 (p<0.0001, OR = 7.0)

CONCURRENT STUDIES FOR STROKE RISK
� Ware, et al. (2003)� CSSCD pediatric patients
� 226 patients, 70 with stroke
� Increased risk: � PAI-1, 4G/4G (p=0.04)
� FVII 37bp repeat (p=0.07)
� Protection:� α-thal (p=0.0019)
� Angiotensin 196 bp allelle (p=0.0084)

STROKE RISK IN SCD
� Sebastiani et al (Nature Genetics, 2005)
� 1398 patients with SCD from CSSCD
� 92 with stroke, 1306 without stroke
� 108 SNPs in 80 candidate genes
� Bayesian networks to analyze gene-gene interactions and their interplay with clinical variables including Hb F and α-thalasemia

STROKE RISK IN SCD
� Sebastiani et al (Nature Genetics, 2005)
� 11 genes were found to interact with Hb F levels to modulate the risk of stroke
� SNPs in 4 genes highly significant
� TGFBR2
� TGFBR3
� BMP6
� SELP (P-selectin)
� Model validated in a different population with a 98.2% predictive accuracy

ASSOCIATION OF SNPs WITH STROKE IN SCD
SNP EFFECT REFERENCE
VCAM1 G1238C Protective Taylor et al,2002
VCAM1 T-1549C Permissive Hoppe et. al, 2004
IL4R S503P Permissive Hoppe et al, 2004
TNFα -308 Protective Hoppe et al, 2004
LDLR/Nco1 Protective Hoppe et al, 2004
ADRB2 Q27E Protective Hope et al, 2004
HLA loci Both Hoppe et al, 2002
BMP6 Permissive Sebastiani et al, 2005
TGFBR2 Permissive Sebastiani et al, 2005
TGFBR3 Permissive Sebasiani et al, 2005
P-Selectin Permissive Sebastiani et al, 2005

TCD

GENETIC RISK FACTORS FOR STROKE
� Phenotype: High TCD (>200 cm/sec)
� Sample Size:
� 230 high TCD (high risk)
� 400 normal TCD (<170 cm/sec, low risk)
� Candidate gene approach (28 polymorphisms)
� Pooled DNA analysis for genome wide SNPs
� Method: High throughput genotyping with MALDI-TOF

Stroke Risk in SCDSNP ODDS RATIO
(95% CONFIDENCE LIMITS)P
adcy9 1.074 (0.723, 1.596) 0.72
apoe 0.943 (0.626, 6.416) 0.77
esell554p 2.741 (0.857, 8.768) 0.084
esels128a 0.699 (0.310, 1.578) 0.38
eselg98t 0.699 (0.310, 1.578) 0.38
fibc148t 0.810 (0.484, 1.357) 0.42
fibg455a 0.652 (0.317, 1.339) 0.24
fva485l 0.948 (0.639, 1.406) 0.79
fviia353g 1.117 (0.694, 1.799) 0.65
fxiiiv34l 0.952 (0.625, 1.451) 0.82
glyc807t 1.065 (0.722, 1.571) 0.75
gp1bt161m 0.716 (0.483, 1.061) 0.095
glyl33p 0.657 (0.397, 1.086) 0.098
icamg241a 0.550 (0.196, 1.543) 0.25
lselp206l 0.730 (0.476, 1.119) 0.15
metht 1.609 (0.956, 2.709) 0.073
pai1 0.846 (0.568, 1.259) 0.41
tgfbr3 0.735 (0.498, 1.086) 0.12
tnfg308 1.126 (0.729, 1.742) 0.59
throma455v 0.775 (0.380, 1.579) 0.48
vcamg1238c 0.601 (0.375, 0.962) 0.032

Catheter Induced
Thrombosis

R485K POLYMORPHISM AND CATHETER INDUCED THROMBOSIS
61-/-
23-/+
26+/+
CONTROL
n=10
THROMBOSIS
n=10R485K
p=0.006 Odds Ratio=4.9

PITFALLS OF GENETIC ASSOCIATION STUDIES
� Small sample size
� Borderline p values or OR
� Unclear phenotypes
� Errors in Genotyping
� Volume of data and what does it all mean?
Ioannidis, et al. Nature Genetics 2001
Lohmueller et al. Nature Genetics 2003

RECOMMENDATIONS FOR
ASSOCIATION STUDIES
� Clearly defined phenotype
� Large sample size (collaborative, multicenter studies)
� Two studies with p<0.01 or a single study with p<0.001
Ioannidis, et al. Nature Genetics 2001
Lohmueller et al. Nature Genetics 2003

IS THERE CLUSTERING OF CLINICAL COMPLICATIONS IN SCD?
� Study of Jamaican patients with a Bayesian model
� 244 subjects (78%) classified into two groups with 95% confidence interval
� Group I – Frequent VOEs, dactylitis, meningitis/sepsis, ACS, and stroke
� Group II – Frequent leg ulcers and anemia
� Splenic sequestration, hypersplenism, and gallstones not linked to either group
� Hb F lowest in Group I; Hb lower in Group II
Alexander, et al. BJH, 126, 606-611, 2004

ARE THERE TWO DISTINCT SUBPHENOTYPES OF SCD?
� Hemolysis/Endothelial cell dysfunction:� Pulmonary Hypertension
� Priapism
� Leg ulcers
� Stroke?
� Vaso-occlusion/hyperviscosity:� Painful episodes
� Osteonecrosis
� Acute chest syndrome
Gladwin & Steinberg

SUBPHENOTYPES OF SCD
Kato, Gladwin, and Steinberg.Blood Reviews, 21, 37-47, 2007

DOWNSTREAM EFFECTS OF HEMOLYSIS IN SCD
Kato, Gladwin, and Steinberg.Blood Reviews, 21, 37-47, 2007

ASSOCIATION STUDIES IN SCD: CONCLUSIONS
� TGFβ/BMP pathway has emerged as an important modifier of SCD severity
� This pathway regulates a wide range of cellular functions (cellular proliferation, differentiation, tissue repair, immune regulation)
� Klotho (KL) has also emerged as a recurrent theme in genetic modulation of SCD
� KL encodes a transmembrane protein with actions on a wide range of cellular processes (antioxidative defense, atherosclerosis, NO metabolism, aging)




TGF-β SUPERFAMILY
� Major signal transduction pathway present in many tissues and cell types
� Comprises ~30 proteins in vertebrates� Regulates diverse cellular functions:
� Cell proliferation� Apoptosis� Response to tissue injury� Bone homeostasis� Inflammation� Immune regulation

DISEASES ASSOCIATED WITH MUTATIONS IN TGF-β PATHWAY
� Hereditary hemorrhagic telangiactasia
� Primary pulmonary hypertension
� Hereditary nonpolyposis colon cancer
� Juvenile polyposis syndrome
� Persistant mullerian duct syndrome
� Diabetic nephropathy
� Sickle cell disease?

CONCLUSIONS
� Genetic modulation of SCD is complex and likely involves multiple gene-gene interactions
� Emerging picture of the phenotypic heterogeneity in SCD is similar to that of complex “multigenic”diseases (CVD, Cancer)
� Elucidation of the mechanisms and pathogenesis of the phenotypic heterogeneity will be possible with a better understanding of the functional effects of the genetic polymorphisms
� Only with this information will it be possible to design novel therapies targeting genetic alterations

MCG Sickle Cell Center: FACULTY AND STAFF
� Adult ClinicAbdullah Kutlar, MD
Kavita Natarajan, MBBS
Celalettin Ustun, MD
Lisa Daitch, PA-C
Sabine Fields, RN
Chakira Brown
Kelvin Jackson
Marva Hall, RN
Chartara Gilchrist, BSW
� Pediatric ClinicVirgil C. McKie, MD
Kathleen M. McKie, MD
Beverly Blanchard, LPN
Atlee Goodwin, RN
� Research Coordinator
Leigh Wells, MSN
Pritam Bora
� Sickle Cell Center LaboratoryFerdane Kutlar, MD
Niren Patel, MBBS
Brian Zhang, MD/PhD
Tao Li, MD
Chinwe Obiaga
� AdministrationAbdullah Kutlar, MD Betsy Clair
















![Prenatal Screening for Co-Inheritance of Sickle Cell ... · Sickle cell anemia and β-thalassemia are genetic disorders caused by different genetic mutations [11]. Therefore, patients](https://static.fdocument.org/doc/165x107/5f5a186f300c56026200ab34/prenatal-screening-for-co-inheritance-of-sickle-cell-sickle-cell-anemia-and.jpg)