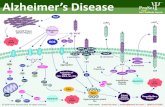
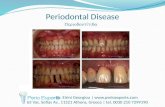
Introduction to Hygiene HEPM 1 RNDr. Sylva Rödlová, Ph.D Institute of General Hygiene.
Ασυνήθεις λοιμώξεις υπεζωκότα€¢ poor oral hygiene,underlying lung...
Transcript of Ασυνήθεις λοιμώξεις υπεζωκότα€¢ poor oral hygiene,underlying lung...

Ασυνήθεις λοιμώξεις υπεζωκότα
Ελένη ΦανιάδουΕιδικευόμενη Πνευμονολογίας
Πνευμονολογική Κλινική ΑΠΘ
ΓΝΘ «Γ.ΠΑΠΑΝΙΚΟΛΑΟΥ»

ΕPIDEMIOLOGY•Pleural infection is one of the oldest and severest diseases
Drainage of the pleural cavity was attempted by Hippocrates over 2,000 years ago to treat empyema
•During the influenza pandemic of 1917–1919, closed pleural drainage became widely practiced to treat postpneumonic empyema
•Up to 57% of patients with pneumonia may develop a pleural effusion
•It can affect any age group, sex and ethnicity and over 65,000 patients suffer from a pleural infection each year in the UK and USA
•The incidence of empyema is rising in both developed and developing countries, including paediatric populations

Parapneumonic effusion is any pleural effusion secondary to
pneumonia (bacterial or viral) or lung abscess
Pleural infections
complicated parapneumonic effusion
for which an invasive procedure, Empyema is, bydefinition, pus in such as tube thoracostomy is necessary, the pleural space.
positive Gram stain or positive bacterial cultures
a process that transforms a ‘simple’ selfresolving parapneumonic pleural effusion into a ‘complicated’ multiloculated fibrinopurulent collection associated with clinical
and/or biochemical features of sepsis.

PATHOGENESIS
1.simple exudate• low white cell count• LDH level less than
half that in the serum • normal pH and
glucose level• sterile
2.fibrinopurulent stage• fluid accumulation • bacterial invasion accelerates
the immune response • further migration of
neutrophils• activation of the coagulation
cascade leading to increased
procoagulant and depressed fibrinolytic activity.
3.organising stage with scar tissue formationFibroblasts proliferatefibrous pleural peel begins to formimpairinglung functioncontinuons potential for infection

• almost half of infected pleural effusions turn out to be microbiologically negative.
• positive culture tests in only 30–40% of cases of pleural infection
inoculation of pleural fluid into blood culture bottles (besides conventional aerobic and anaerobic culture) might increase sensitivity by about 20%• The First Multicenter Intrapleural Sepsis Trial (MIST1) assembled
a large, well-characterized patient cohort
screen for bacterial pathogens from pleural fluid samples by the amplification and sequencing of the bacterial 16S ribosomal RNA gene which has been shown to improve the identification of pathogens from cases of pleural infection

Biochemical sampling of the pleural fluid is essential.
Neutrophil phagocytic activity, with protease production leads to a fall in pH of the pleural fluid fall in glucose, both characteristic biochemical
features of complicated parapneumonic effusions and
empyema.
A rise in lactate dehydrogenase often in excess of three times the upper
limit of normal.
Pleural fluid glucose correlates with pH and can be an
alternative if accurate pH analysis is not available.
Many other biomarkers have been investigated for the
diagnosis of pleural infection from simple parapneumonic
effusions or effusions of other aetiologies,. procalcitonin
e.g
DISTINGUISING COMPLICATED FROM UNCOMPLICATED PLEURAL EFFUSION

• Community-acquired infection • Hospital-acquired pneumonia • Post–thoracic surgery(especially lung resection)• Post-traumatic thoracic (open or closed) trauma • Post–abdominal surgery• Oesophageal rupture• Spontaneous bacterial pleuritis• Lung cancer associated empyema• Iatrogenic (after insertion of chest tubes)• Unclassified• It is possible that genetic predisposition contributes to
development of empyema.
ETIOLOGY

• Vary according to the underlying infection• in the UK-based Multicentre Intrapleural Sepsis Trial
(MIST) of 430 patients,• the median (interquartile range) duration of symptoms
prior to• recruitment was 14 (8–28) days • Aerobic pneumonic infections will tend to present with an
acute febrile illness, localised pleuritic chest pain, sputum production and leukocytosis.
• Anaerobes tend less pronounced fever and systemic symptoms, such as poor appetite and weight loss, anemia
such infections are more common in those with poor dental hygiene, in alcoholics and in danger of aspiration of gastric contents
CLINICAL MANIFESTATIONS

RISK FACTORS• Young• Male• diabetes mellitus• immunosuppression
gastrooesophageal reflux disease• aspiration • alcohol abuse • Intravenous drug abuse• smoking• Poor dental hygiene appears to
be a risk factor for anaerobic infection
• COPD might be protective
Steroids have potent effects on attenuating pleural inflammation

John P Corcoran et alLancet Respir Med 2015; 3: 563–77
MECHANISMS

• Important to separate pleural infections community-acquired pneumonia hospital-acquired cases and iatrogenic
aetiology, for example, following thoracic surgery
as the causative bacteria are often different.
• Hospital-acquired empyema has a significantly worse outcome, with a mortality of up to 50% and must be treated urgently and aggressively.
• Age-dependent variation higher rate of
S pneumoniae (up to 85%) and Streptococcus pyogenes in children
geographical variation occurs
in Asia where Klebsiella pneumoniae is often the most common pathogen, causing up to 25% of cases• one-year mortality values varied
depending on bacterial subtype: 17% Streptococcal spp 20% anaerobes 45% Gram-negative bacteria, 44% S aureus 46% with mixed aerobic bacteria
MICROBIOLOGY

MICROBIOLOGY
Hospital-acquired infection in adults is most
commonly S aureus(35%) particularly
methicillin-resistant S aureus 18% Entero bacteriaceae 18% Streptococcus spp (7% from the S milleri group, 5%
from S pneumoniae), 12% Enterococcus spp 8% from anaerobes
community-acquired infection in adults is most commonly
streptococcal (52%), 24% the S milleri group
(Streptococcus anginosus-constellatus-intermedius)
21% S pneumonia, 20% anaerobic microbes, 10% S aureus 8% from Enterobacteriaceae
(including Escherichia coli and Proteus spp).

MICROBIOLOGY
• The role of oropharyngeal bacteria in pleural infection
has long been recognised.• Aspiration of these bacteria polymicrobial anaerobic and
facultatively anaerobic bacteria
The S milleri group of bacteria are the most frequent
cause of community-acquired pleural infection.• co-localisation of S milleri and anaerobes in pleural infection• The defective mucociliary clearance ,low oxygen tension
associated with an atelectatic or consolidated lung allow oropharyngeal anaerobes to fourish.
• Despite the high frequency with which atypical organisms
cause pneumonia, mycoplasma pneumoniae and legionella are rarely identified in pleural infection, suggesting an absence of tropism for the pleural space.

• Pulmonary nocardiosis is an infrequent but serious opportunistic infection that commonly presents as a sub-acute or chronic necrotizing pneumonia, mimicking tuberculosis, lung carcinoma or abscess
• Pleural involvement in pulmonary nocardiasis is seen in 25% of cases including pleural effusions and empyema
• Several risk factors such as corticosteroid therapy, chronic obstructive• pulmonary disease (COPD), cystic fibrosis and bronchiectasis, diabetes,
autoimmune diseases, chronic lung disease, chronic granulomatous disease, HIV infection
• Nocardia asteroides complex is the most common • routine search for Nocardia should be done by incubating the cultured clinical
specimens forat least one week.• Rapid and accurate identification of nocardial species is now possible through
molecular techniques –PCR • Treatment TMP-SMX

• Pulmonary actinomycosis often presents with parenchymal disease with less than 2% showing pleural involvement.
• poor oral hygiene,underlying lung disease, alcoholism, and possibly HIV infections.
• It canmimic granulomatous disease, and oftentimes, distinction from tuberculosis,
• fungal infections, or malignancy is problematic.• The classical microscopic appearance of this gram
positivebacillus on cultures• Actinomycotic empyema is treated with prolonged antibiotic
therapy penicillin.tetracyclines to 6-12 months • surgical drainage and decortication

• Rickettsia are a group of small, pleomorphic, Gram negativeCoccobacilli• Rickettsia rickettsii is the most commonly known.• Rocky Mountain spotted fever (RMSF) fever, headache, and rash• Mediterranean spotted fever(MSF) fever, rash, and eschar• Serology using indirect fluorescent antibody (IFA) (PCR) from skin
biopsies of eschars• The pleural fluid a neutrophil exudate.
• Coxiella burnetii is a small, gram-negative intracellular• bacteria of Q fever. It is a zoonotic• febrile illness with acute and chronic presentations • Q fever is known to cause atypical pneumonia • IgM and IgG antibodies Immunofluorescence assay serology• PCR DNA• pleural fluid which an exudate with• marked eosinophilia

fungal infections increasing use of broad-spectrum antibiotics,
intravascular devices, critically ill or immunocompromised patients
The diagnosisof bronchopulmonary infection difficult to confirm: because fungi isolated from sputum may represent either pathogens or saprophytes,
invasive diagnostic procedures such as bronchoscopy or lung biopsy are usually necessary
1.isolation of a fungal species from
the pleural effusion belonging to the exudate category, according to
the criteria of Light et al15
2. significant signs of infection, such as fever (body temperature . 38.3°C) and leukocytosis (white blood cell . 10,000/mL
3.isolation of the same mold species from pleural effusion on more than one occasion, or from pleural effusion and other specimens such as blood, sputum, or surgical wounds thatshowed evidence of tissue invasion
FUNGAL EMPYEMA

• fungal empyema most often in ICUs• overall mortality up to 73%. • Candida species albicans are the most common pathogens ,a complication of
operation,gastropleural fistula,and spontaneous esophageal rupture• Aspergillus empyema thoracis is uncommon and is caused by rupture of an
aspergillomacavity or as a complication of a preexisting chronic• empyema. • Aspergillus is important to have as a differential in a patient who has had past treatment
with artifical pneumothorax therapy for tubercuslosis The post operative period after pneumonectomies and lobectomies is another situation in which aspergillus is frequently encountered
• Pleural cryptococcosis has been reported
to be associated with HIV infection, and liver cirrhosis,• Gram-stained smear• Cultures• antifungal therapy• decortication because of poorly controlled infection

• With increasing travel and migration, rates of parasitic lung and pleural diseases are increasing in the immunocompetent population in developedcountries as well as among immunocompromised patients
• Amoebiasis is caused by Entamoeba histolytica, a protozoan foundWorldwide• Blood-borne spread formation of an amoebic liver abscess which may present• A serous pleural effusion may occur in conjunction with an amoebic liver
abscess• Amoebic pleuropulmonary disease is the most common• complication of amoebic liver abscess, occurring in 15% of• patients with amoebic liver disease • It most commonly occurs by direct extension from a superior right lobe hepatic
abscess through the diaphragm into the right lower lobe of the lung, presenting with cough, pleuritic pain and dyspnoea.
• Intrathoracic complications include rupture of an amoebic liver abscess into the pleural cavity with empyema
PARASITIC INFECTIONS

• Pulmonary paragonimiasis is most frequently seen in south east• Asia but also occurs in central Africa and South America• Presenting symptoms include pleuritic chest pain, haemoptysis, chronic cough and fever• Peripheral blood eosinophilia total serum IgE may be raised.• The eosinophil counts are usually elevated in pleural and bronchoalveolar• lavage fluids. • The identification of the characteristicoperculated eggs in faeces, sputum or
bronchoalveolar lavage fluid confirms the diagnosis.
• Visceral leishmaniasis (VL) is usually characterized by splenomegaly, pallor and fever. Pleural effusion is an uncommon feature of this disease, in immunocompromised Common pulmonary symptoms in VL are usually related to bacterial lung infection, vagal nerve compression by splenomegaly, and hypoalbuminemia with mild pulmonary edema
• histiocytes containing Leishmania amastigotes in pleural fluid , Bronchial biopsies• aspirate smears• Other parasites, including hydatid disease (Echinococcus spp), fi lariasis• (Wuchereria bancrofti), Toxoplasma gondii ,trichomonas

• extrapulmonary TB serves as the initial presentation in about 25% of adults, and primarily involves the lymph nodes and pleura
• mycobacterial infection within the pleural space• Where HIV is endemic,TB pleuritis is the most common cause of a lymphocytic pleural
effusion• Fever,productive cough,pleuritic chest pain, night sweats, chills, weakness, dyspnoea,• and weight loss• Chronic TB empyema is less common, represents a distinct entity of chronic, active
infection within thepleural space, characterised by purulent fluid where all white blood cells are neutrophils,
• TB effusions are largely unilateral ,a slight right-sided predominance, of cases (Figure 2) The effusions are typically small to moderate in size, occupying less than one-third of the
hemithorax - coexistence of parenchymal disease .
TB PLEURITIS

• The gold standard for the diagnosis of TB pleuritis is detection of M. tuberculosis in the sputum, pleural fluid or pleural biopsy specimens,
either by microscopy and/or culture, • the histological demonstration of caseating granulomas in the pleura (of closed pleural
biopsies, thoracoscopy or open surgical biopsies)along with acid fast bacilli (AFB) is diagnostic.
In populations with a high prevalence of TB and clinical suspicion of TB effusion the diagnosis is frequently inferred in patients who present with a lymphocytic predominant exudate and high ADA level (between 40 and 60 U/L)• Effusion exudative having protein concentrations invariably >30 g/L T• (LDH) level exceeds500 IU/L • The pleural fluid pH is usually less than 7.40 • A low pH and low glucose concentration may be observed but are more
characteristic of chronic tuberculous empyema than TB• The cell count performed usually reveals a nucleated (white) cell count between 1,000 and
6,000 cells/mm3 (29),
75% lymphocytes and/ or a lymphocyte to neutrophil ratio more than 0.75
TB PLEURITIS

• NTM pleurisy has become a clinical concern.• Growth in numbers of elderly and immunocompromised• populations malignancy,AIDS, diabetes mellitus,end-stage renal
disease,cirrhosis of liver • NTM pleurisy patients had higher leukocyte count, lower lymphocyte• percentage and lower total protein level compared to TB pleurisy• MAC remains the most common• Diagnosis:multiple culture-positive PE samples plus pleura histology• showing granulomatous infllammation• NTM pleurisy• 1-year mortality rate of 37%• treatment is associated with better survival
NTM PLEURISY

• Although bacterial pleural infection is associated with epidemics of influenza (eg,the 2009 H1N1 influenza A epidemic was associated with increased rates of
pneumococcal and S pyogenes pleural infection),a few small studies have addressed the direct role of ofcommon respiratory viruses in community-acquired
pleural infection.• Pleural eff usions are associated with o Adenoviruso Hantaviruso Cytomegaloviruso herpes viruses.
The effusion is an exudate and lymphocytes dominate, are often bilateral and are accompanied by a diffuse parenchymal infiltrate typical of a viral pneumonia.
EBV infection/reactivation can account for certain proportions of “idiopathic” effusions (59%) amongst immunocompromised patients with unexplained effusions.
Associated specific B-cell lymphomas such as pyothorax-associated lymphoma
Polymorphous lymphocytosis is the most common cytologic feature
VIRUSES

• SBEM criteria include transudative pleural fluid• in the absence of pulmonary source of infection, with polymorphs>• 500 cell/mm 3 or positive pleural fluid• advanced liver disease, low pleural fluid protein, or SBP are at risk for
spontaneous bacterial pleuritis. • cirrhotic patients with hydrothorax (Escherichia coli, enterococcus and
klebsiella species, suggesting gastro Intestinal source)
• -Empyema in chronic kidney disease/end stage renal disease of aerobic gram-positive organisms while in CKD stage aerobic gram-negative organisms
• antibiotic treatment is the preferred approach• Immuno-compromised state is thought to be• contributing factor in both these cases.
SPONTANEOUS BACTERIAL PLEURITIS-EMPYEMA

• Trauma is an epidemic that is increasing. It causes more
than 5 million deaths per year. Among the types of trauma,• chest trauma is one of the most common disorders that
comes to the emergency. • Post traumatic empyema is rare in patients with chest trauma that occurs
around 1% to 4.2% of Cases• One of the most important risk factors is coagulated hemothorax • blunt trauma -magnitude of the trauma• penetrating chest trauma -direct contamination of the pleural space• The average length of hospital stay in the ICU-A for the group of patients
with chest trauma who developed posttraumatic empyema was 26.7• Empyema management -thoracoscopy in 100% of cases.
POST TRAUMATIC EMPYEMA

• Empyema after TT has a reported incidence of 1% to 25%, depending on the study/population characteristics
• The presence of a pleural effusion prior to tube placement carries a higher risk of empyema
• Staphylococcus aureus is the most frequent organism associated with empyema.
• Treatment include continued TT drainage, new tube placement, image-directed drainage, intrapleural fibrinolytic therapy, thoracoscopy, and open pleural decortication.
THORACOSTOMY TUBES

Post-pneumonectomy empyema (PPE) is an uncommon yet serious complication,
In general, the incidence is between 2% and 16%.
Post-pneumonectomy empyema may be classified into simple
or complicated types.
The latter is associated with a fistula, most
commonly BPF• Staphylococcus aureus• Pseudomonas aeruginosa
Aim:
control the sepsis and its sequelae• optimize residual lung function • provide appropriate• ventilatory support and • nutritional supplementation as necessary• clear out pleural cavity infection and achieve the• closure of BPF if present. Closure of BPF is particularly important
because it removes the source of contamination and prevents
aspiration to remaining lung.

• The diaphragm is normally an effective barrier to the spread of Infection• 15 per cent of subdiaphragmatic abscesses are complicated by empyema• diagnosis of empyema should be considered in any patient with• sudden onset of respiratory distress who has previously
undergone abdominal surgery or had recent abdominal pain,
particularly if there are signs of a pleural effusion. • differentiated from pulmonary thrombo-embolism and basal pneumonia
• perforated duodenal• ulcer• Small bowel• Obstruction• Appendicitis• appendicectomy• septic splenic infarction• Acute pancreatitis• cholecystojejunostomy
INTRAABDOMINAL SEPSIS

• Empyema is a rare but recognized complication in patients with CF. • In these patients the causative organisms have been reported to be • S. aureus,• P. aeruginosa• Burkholderia cepacia• Ps. aeruginosa• Empyema CF on long-term oral corticosteroid• therapy due to treatment of allergic bronchopulmonary• aspergillosis (ABPA)• inflammatory response contributes to lung destruction over time, may be
a protective mechanism in terms of extrapulmonary spread of bacteria• pre-and post-transplantation immunomodulator therapy
and chronic corticosteroid use have been hypothesized as
predisposing causes leading to empyema in several cases
EMPYEMA AND CYSTIC FIBROSIS

• Human immunodeficiency virus (HIV) infection is a risk factor for empyema,• Common pathogens:• include S. pneumoniae, Staphylococcus aureus, S. anginosus,• S. pyogenes, Prevotella spp. and M. tuberculosis• S. aureus and enteric Gram-negative organisms occur more frequently• Gram-negative organisms occur more often in HIV-infected
non-typhoidal Salmonella is well described in patients with advanced HIV• Pseudomonas aeruginosa and Acinetobacter baumannii as contact with health
facilities• In southern Africa, the majority of patients with tuberculosis• empyema are HIV infected• However, pleuropulmonary complications are rare, with• empyema usually occurring in the setting of CD4 counts• < 100 cells/mm• Patients on ARV therapy had significantly shorter lengths of stay.
HIV AND EMPYEMA

• Pleural effusions occur in 25% of patients within the first 90 days after lung transplantation• The predominant organism cultured from the pleural fluid was Candida albicans, which• accounted for 44% ,nosocomial pathogen in the intensive care unit (ICU). • Fungal species caused 61% (n=22) • bacterial species were responsible for 25% (n=9) of the cases, gram negative pathogens.
Atypical causes of pleural infection included Mycoplasma hominis (n=2) and Mycobacterium tuberculosis.
• An increased pleural LDH and particularly an increased• neutrophil percentage among the total pleural cells is highly predictive indicator of pleural• Early pleural space infection thus identifies patients at increased risk for additional• complications and one year mortality• increased risk for pleural infection in bilateral as compared to single lung transplantation No
significant differences were observed in • age,• gender,• native disease,• type of transplant operation
ΤRANSPLANTATION AND EMPYEMA

Empyema associated with primary lung cancer is rare,
and its incidence ranges from 0.1% to 0.3% (2, 4).
It may be considered to be associated with natural complications of
cancer, immunosuppression status, consequences of pneumonia
and necrotic tissue following chemoradiotherapy or
invasive procedures
pleural fluid should be conducted,
including erythrocyte/leukocyte counts, gram staining, cultures,
and cytological examinations
LUNG CANCER RELATED EMPYEMA

• Sepsis• pleural fibrosis may develop (fibrothorax).• Pleural calcification,• bronchopleural fistula formation • development of empyema necessitans (disruption of the parietal• pleura with spontaneous discharge of pleural contents evident
under the chest wall) • Pleural lymphoma is rare. It may arise in approximately 2% of
patients with a long-standing pyothorax (>20 years), usually• following induction of an artificial pneumothorax for
tuberculosis.• association with EpsteineBarrvirus infection
COMPLICATIONS

• low serum albumin 30 g/l,• elevated C-reactive protein (CRP) .100 mg/l • platelet count .400 109/l,• low serum sodium 130 mmol/l,• intravenous drug use or chronic alcohol abuse were all were• identified as independent predictors of the subsequent development• of complicated parapneumonic effusion or empyema. • chronic obstructive pulmonary disease (COPD) was• associated with decreased risk complicated parapneumonic effusion
• empyema can be predicted by deriving a scoring system with• good predictive value. The presence of >2 of the above risk• factors has a 87% sensitivity for detection of complicated• parapneumonic effusion or empyema
PREDICTING FACTORS

Categorizing Risk for poor Outcome in Patients with Parapneumonic Effusions and Empyema
Parapneumonic Effusions and EmpyemaRichard W. Light

• Pulmonary embolism (PE),• bronchial/pleural malignancy, lung abscess • collagen vascular diseases and• iatrogenic causes (drugs) can all mimic pleural space infection• Pleural sepsis secondary to oesophageal rupture can be confused with
primary empyema, especially in the elderly or if there is no clear history of chest pain or vomiting. amylase of salivary origin chylothorax or pseudochylous effusion can also lead to clinical confusion and thus, the aspirate should be analysed for the presence of cholesterol and triglycerides
• In pancreatitis, pleural fluid analysis may demonstrate raised amylase, and isoform analysis may be used to confirm pancreatic rather than salivary origin.
• Rheumatoid pleuritis the pleural fluid may be acidic, with low glucose levels. In these cases a history of joint disease and RhF positivity may lead to the diagnosis
DIFFERENTIAL DIAGNOSIS

• Parapneumonic Effusions and Empyema - Richard W. Light• The Bacteriology of Pleural Infection by Genetic and Standard
Methods and Its Mortality Significance - Nick A. Maskell, Sarah Batt, Emma L. Hedley
• BTS Pleural Disease Guideline 2010 • Pleural effusion as the initial clinical presentation in disseminated
cryptococcosis and fungaemia: an unusual manifestation and a literature review - Mayun Chen, Xiaomi Wang, Xianjuan Yu
• Diagnosis and Outcome of Early Pleural Space Infection Following Lung Transplantation - MM Wahidi, DA Willner, LD Snyder
• Tuberculous pleural effusions: advances and controversies - Morné J. Vorster, Brian W. Allwood
• Fungal Empyema Thoracis An Emerging Clinical Entity - Shiann-Chin Ko, Kuan-Yu Chen
References

Σας Ευχαριστώ για την προσoχή σας!